Chronic thromboembolic pulmonary hypertension (CTEPH) is a severe form of pulmonary hypertension that develops in some patients who have suffered a pulmonary embolism, when the thrombi causing the blockage do not disappear. The mechanisms responsible for it have not yet been clarified. Given the important role of endothelial cells in the regulation of vascular function, malfunctioning of these cells could explain the development of CTEPH after a pulmonary embolism.
For the purpose of corroborating said hypothesis, researchers from the Hospital Clínic-IDIBAPS Physiopathological Mechanisms of Respiratory Illnesses group and from the CIBERES, led by Joan Albert Barberà, analysed endothelial cells obtained from material extracted during pulmonary endarterectomy, the treatment of choice for CTEPH. In this complex surgical procedure, the thrombotic material and endothelial layer of the obstructed pulmonary arteries are removed. This material offers a unique opportunity for the direct study of pulmonary endothelial cells.
“In the study, we observed that pulmonary endothelial cells of patients with CTEPH are more proliferative and show less apoptosis than control cells. Furthermore, they have less capacity for migration and formation of new blood vessels”, comments Olga Tura-Ceide, the first author of the article and researcher at the Hospital Clínic-IDIBAPS, as well as the Biomedical Research Institute of Girona (IDIBGI). “We also observed that the endothelial cells of these patients present an altered molecular signature, with overexpression of molecules of adhesion, high levels of oxidative stress and mitochondrial anomalies”, points out Valerie Smolders, also the first co-author of the article.
“The relevance of the article is twofold,” comments Barberà. “On the one hand, we have identified molecular pathways that could influence the lack of resolution of thrombi, the remodelling of the vascular wall and the development of CTEPH and, consequently, they could constitute new biomarkers and therapeutic targets for the disease. On the other, we now have an in vitro model of pulmonary endothelial cells from several dozen patients with CTEPH which will enable us to conduct future studies with drugs specifically aimed at correcting the alterations observed”.
The study has been financed with funds originating from the European Union (BIOTRACK-Marie Curie programme), the Carlos III Health Institute, the CIBERES Pulmonary Hypertension Line and the Foundation Against Pulmonary Hypertension.
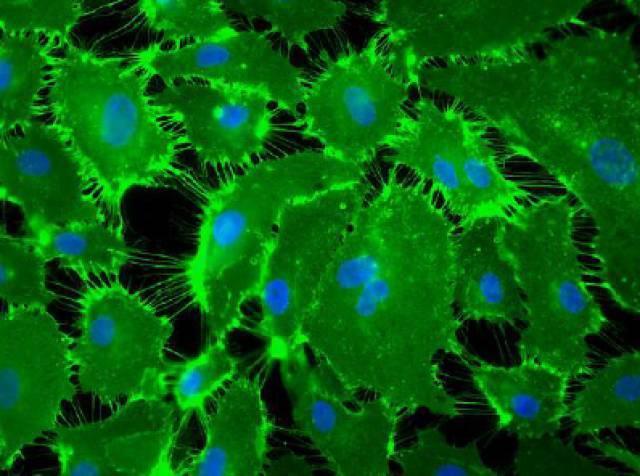
Fluorescence image showing overexpression of adhesion protein and endothelial marker (CD31, in green) in endothelial cells derived from patients with CTEPH. In blue, nuclei marked with DAPI. Magnification x10.
Reference
Tura-Ceide O, Smolders VFED, Aventin N, Morén C, Guitart-Mampel M, Blanco I, Piccari L, Osorio J, Rodríguez C, Rigol M, Solanes N, Malandrino A, Kurakula K, Goumans MJ, Quax PHA, Peinado VI, Castellà M, Barberà JA. Derivation and characterisation of endothelial cells from patients with chronic thromboembolic pulmonary hypertension. Sci Rep. 2021 Sep 22;11(1):18797. doi: 10.1038/s41598-021-98320-1.




