The Hospital Clínic-IDIBAPS is making progress in its approach to cluster headache through the deep brain stimulation of patients as compassionate treatment. This is an infrequent disease with few cases published in scientific journals that do not respond to the usual treatments. The first patient treated with the Hospital Clínic’s improved technique was in Spain, and fewer than 10 patients have been treated with it worldwide. The implantation of electrodes that stimulate and modulate brain activity had already been carried out in other cases, but it had not been possible to monitor brain activity simultaneously to try to detect new episodes before the patient noticed them. Knowing the possible patterns that precede and predict an episode could improve treatment, reducing the possible harmful effects on the brain. Three months after the operation, the patient’s quality of life has improved, from 5 suffering headache episodes a day to none or sporadic and mild episodes that do not require treatment The cluster headache is known as the “suicide headache" due to the fact that these sudden episodes of very intense pain have an impact on the patient's quality of life, becoming a risk factor for suicide.
This is an infrequent disease with few cases published in scientific journals that do not respond to the usual treatments. The first patient treated with the Hospital Clínic’s improved technique was in Spain and fewer than 10 patients have been treated with it worldwide.
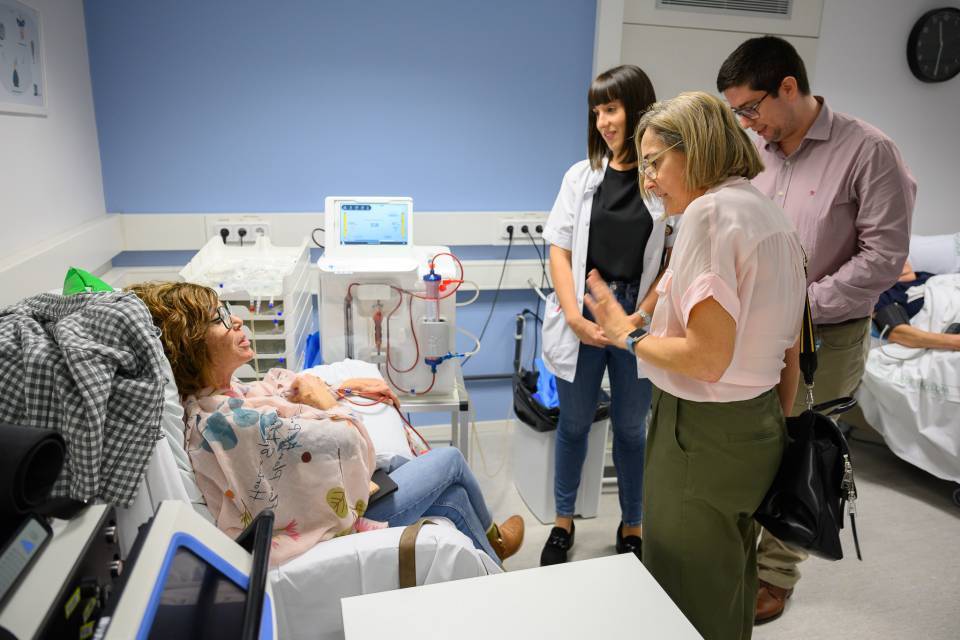
The Hospital Clínic has carried out the neurostimulation of patients as compassionate treatment, co-directed by Dr. Víctor Obach and Dr. Santiago Fernández, neurologists, and Dr. Pedro Roldán and Dr. Jordi Rumià, neurosurgeons. They are all members of the multidisciplinary ‘Headache and Facial Pain’ group led by Dr. Neus Fabregat, from the Hospital Clínic Neurosciences Institute of the Hospital Clínic Barcelona. The patient presented with a cluster headache refractory to the usual treatments. The results of this first case were successful. The 58-year-old patient presented with 3-5 episodes of intense headache (1-2 episodes were nocturnal), which lasted 30-60 minutes, with no response to any treatment over the last 10 years. Since brain stimulation, he has not had any more episodes or required rescue medication. He has been able to sleep again, regaining the desire to carry out personal and family activities that he had abandoned, such as riding motorbikes. Moreover, the implanted electrodes have begun to record his brain activity and it is hoped that we will soon obtain important data that will allow any possible future episodes to be predicted. Thus, it is hoped that brain stimulation can be discontinuous and that it will only be carried out when a possible crisis is detected. It will also reduce the possible side effects on the brain and its connections, and extend the life of the battery in the implanted generator.
The electrodes were implanted in the ventral tegmental area, near the hypothalamus, in an operation that lasted 3 hours and 4 hours in the ICU, with no immediate complications. Three days later, the patient was discharged and chronic stimulation began on day 21, after the implantation of the electrodes and the verification of their correct placement and functionality. After the first few weeks of stimulation, unpleasant side effects attributable to the stimulation were ruled out.
The cluster headache
Cluster headache is one of the most painful types of headache, alongside trigeminal neuralgia. Although it is infrequent, it is the second most common primary headache after migraine. In Spain, it is suffered by around 47,000 people, being more frequent in men than women. Twenty per cent of current cluster headaches are considered chronic, and 10% of them do not respond to conventional treatment. At the Hospital Clínic, 70 patients have been followed up over the last 10 years.
The main symptomatology is sudden episodes of very intense and totally disabling pain in the same part of the face and eye, almost always on one side, which generally last between 30 minutes and 3 hours at any time of the day or night. Moreover, they are accompanied with other signs in the eye region such as tearing of the eye and drooping of the eyelid, as well as a stuffy or runny nose, all on the same side as the pain. The episodes tend to have a circadian and seasonal predisposition. In other words, they usually occur at specific times of the day and in specific months of the year, with no symptoms outside of these periods.
There are different types of treatment for these headaches, depending on the time of the onset and the chronicity of the disease. Some of the main symptomatic treatments are triptans, preferably in their injectable or nasal spray forms, and oxygen. Corticosteroids and lidocaine are also administered through greater occipital nerve infiltration. Moreover, verapamil in tablet form is also used as preventive treatment.
When the patient does not respond to these treatments and to other less established ones such as botulinium toxin, other more invasive techniques are considered such as anaesthetic block or sphenopalatine ganglion electric radiofrequency. Deep brain stimulation is an alternative that is still being studied and has been used in very few cases worldwide. During episodes, it is also recommended to avoid triggers such as alcohol consumption.
Clínic Barcelona’s experience with deep brain stimulation
Deep brain stimulation is a technique indicated for movement disorders such as Parkinson’s disease, dystonia or essential tremor, which are refractory to conventional treatment. More recently, it was also approved for use in refractory epilepsy and other neuropsychiatric disorders.
The Hospital Clínic Barcelona is a national referral centre for this type of disorder, with over 300 interventions with very good results: no mortality and less than 0.5% of surgery-related infections and reoperations due to side effects or complications. The Hospital has over 25 years of experience in deep brain stimulation in movement disorders, over 5 years in refractory epilepsy and over 2 years of experience in other neuropsychiatric disorders.
With the recent incorporation of deep brain stimulation in cephalalgia, the aim is to further expand the possible indications of this technique. Furthermore, we are trying to improve the technique by reducing the possible side effects of electrical toxicity by limiting stimulation to specific moments through data collection.