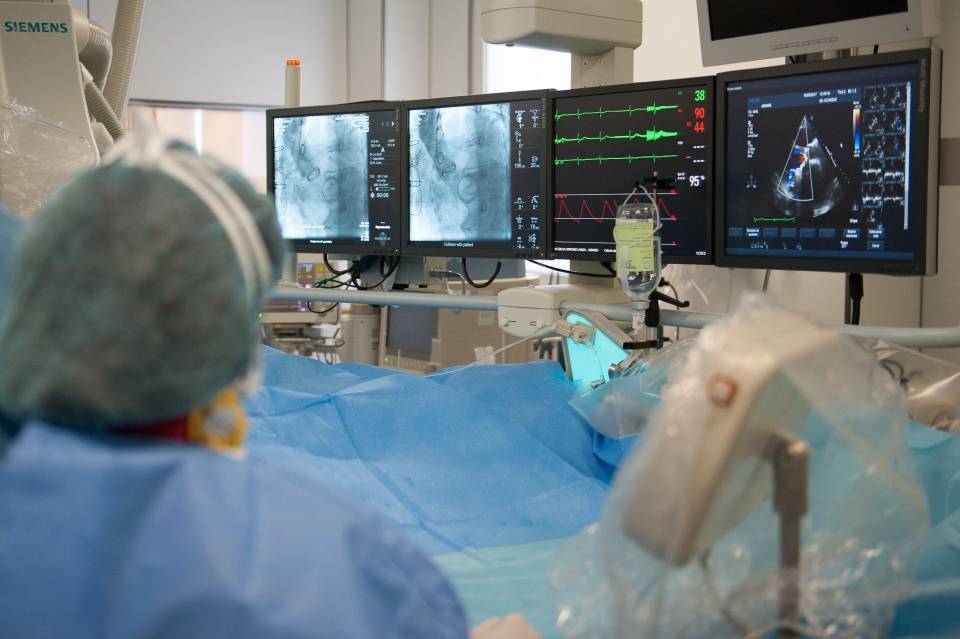
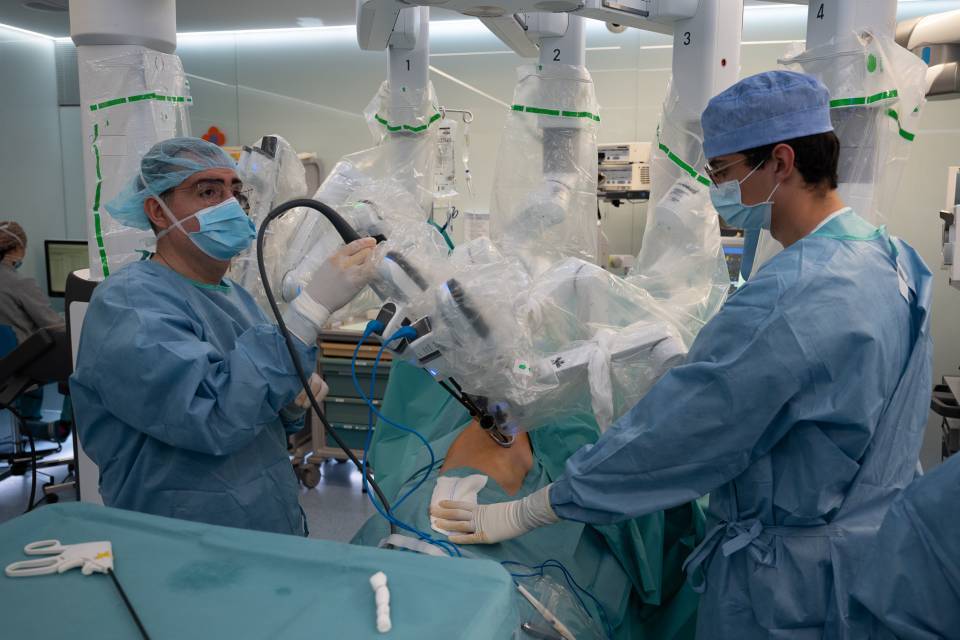
Atrial fibrillation (AF) is one of the most common arrhythmias, especially among the elderly, occurring in the left atrium. In addition, it increases the chances of suffering an embolism and, therefore stroke, from a clot or thrombus created in the left atrium that will travel to the brain.
Recently, a team of physicians and researchers from the BCN Medtech Unit at UPF, Hospital de la Santa Creu i Sant Pau and Hospital Clínic de Barcelona, have corroborated that analysing the patient's blood flow by means of simulation can help improve monitoring the problem or determine whether closer patient follow up is needed. The research has recently been disseminated in the form of two scientific articles published in Revista Española de Cardología and in Mathematics.
Until a few years ago, the main treatment for this condition was based on anticoagulant pills that patients had to take every day, for ever. Aside from the inherent problems, many of those affected could not take these pills due to other illnesses or contraindications to treatment due to the risk of bleeding.
Currently, there is a surgical alternative called left atrial appendage closure. “It is a minimally invasive intervention that closes the left atrial appendage, the cavity where the thrombus forms, thanks to the placement of a small device that seals its contents”, explains Jordi Mill, first author of the research and researcher with the UPF BCN Medtech Unit. He adds that “it is a good alternative as, the same or the next day, the patient can return to normal life and need no longer take anticoagulants”.
Despite this, “some of these patients operated on develop thrombi on the surface of the installed device and, therefore, continue to have the problem we wish to avoid”. To resolve this, a study was conducted that analysed differences in blood flow pattern in three patients who had developed a thrombus due to the installation of the device and in three patients who had not.
The medical community believed that the cause of the problem was the way in which the device is positioned, since, depending on the orientation it favours areas of blood flow stagnation and low-speed recirculation that would trigger the thrombus formation process. This theory, however, “is difficult to verify with current medical images because they are not of sufficiently high resolution to detect these flow patterns near the implanted device”, Jordi Mill comments.
The differences in blood flow pattern found between the two groups, through the simulations, have been quite clear and have corroborated the hypotheses held by the physicians: certain positions of the device favour flow recirculation and stagnation at low speeds and, therefore, the risk of thrombus formation.
Dr. Dabit Arzamendi, from the Department of Cardiology of the Hospital de la Santa Creu y Sant Pau, remarks that "this study can have an important clinical impact to improve the subsequent treatment that patients will receive". Despite this, Dr. Xavier Freixa, from the Department of Cardiology at Hospital Clínic explains that "we will need more extensive series to better understand the findings of this first study."
For practical purposes, Mill asserts, “this study reveals two relevant findings that can greatly improve the resolution of the problem; on the one hand, performing personalized flow simulations for each patient before undergoing the operation, to judge the best position for the device, and on the other hand, to apply simulations after the operation, in cases where the device has remained in a position that risks forming a thrombus, to determine whether there is a need to follow up the patient more closely”.
Reference works:
Mill, J. Et al. (2021, September). Sensitivity Analysis of In Silico Fluid Simulations to Predict Thrombus Formation after Left Atrial Appendage Occlusion. Mathematics. DOI:10.3390/math9182304
Mill, J. Et al. (2021, July). Patient-specific flow simulation analysis to predict device-related thrombosis in left atrial appendage occluders. Revista Española de Cardiología. DOI: 10.24875/RECICE.M21000224