AMD is the primary cause of irreversible vision loss among the population over 60 years. It is estimated that there will be around 196 million people with AMD worldwide by 2020. Local inflammation and immune-mediated processes play a crucial role in the development of this disease. The analysis of ocular drusen –cellular debris deposits that accumulate under the retina and which are characteristic of AMD– shows that these deposits contain inflammatory proteins and other components that contribute to local inflammation process. Among them, the C-reactive protein (CRP) –involved in the regulation of the innate immune system and a biomarker of chronic inflammation; cardiovascular disease and AMD– is found. "Although the C-reactivate protein has been detected in drusen and in other deposits in the retina, little is known about its role in the context of AMD," explains Dr. Molins. "In addition to CRP, there are other AMD risk markers. Among them it is found a polymorphism (Tyr402His) in the gene for complement factor H (FH) and it increases from 5 to 8 times the risk of AMD in homozygous individuals, i.e. those having two identical copies of this gene in homologous chromosomes", she adds.
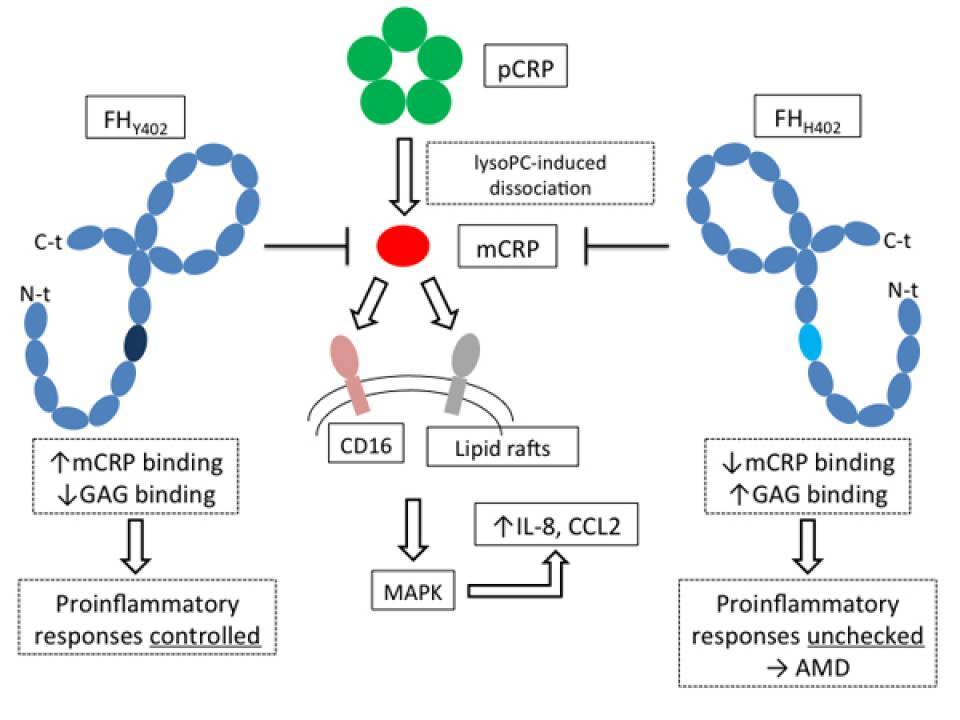
The article published in Scientific Reports provides new information of the CRP contribution to the development and progression of AMD. In plasma, CRP exists as a pentamer which in presence of damaged cells or certain substances, can dissociate into smaller subunits. Researchers have performed studies in retina cell lines and have identified that the CRP subunits, and not the plasmatic form, are the responsible for inducing an inflammatory response that may contribute to the progression of AMD. Authors have also shown that FH variant associated with AMD risk defectively binds to the monomeric form of the CRP and is not able to prevent its proinflammatory activity. Instead, the FH variant not associated with this risk binds efficiently to mCRP and prevents proinflammatory activity. In this way the authors describe a new mechanism of AMD pathophysiology.
Article reference:
Molins B, Fonts-Prior P, Adan A, Antón R, Arostegui JI, Yagüe J, Dick AD.
Sci Rep. 2016 Mar 10; 6: 22889. doi: 10.1038 / srep22889.