Less than two years after the first uterus transplant at the Hospital Clínic, the team led by Dr. Carmona and Dr. Alcaraz carried out a second transplant. This time, it was possible thanks to a mother donating her uterus to her daughter, and the 18-hour operation was a success. Two months after the procedure, the patient had her first menstrual period, and it is hoped that the first embryo can be implanted at the end of this year.
Changes compared to the first operation and after the transplant
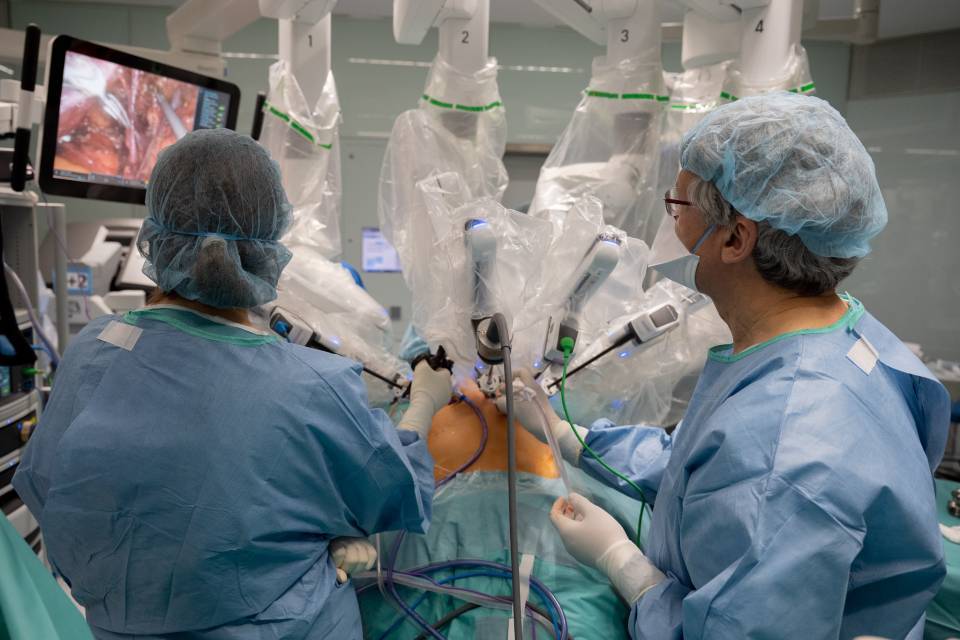
Several technological modifications were made in this second operation in comparison with the first transplant. The team used an exoscope. This is a new device that the hospital incorporated a few months ago and consists of a high-magnification lens that produces high-definition images. This device has helped in bench surgery, when the uterus is removed from a patient’s body and is being prepared for transfer, and in the implantation in open surgery.
Moreover, the number of viable embryos has also been changed. The patient who received the first transplant had her first menstrual period one-and-a-half months after the operation, but has still not achieved a viable pregnancy. At that time, 4 healthy embryos were available, but this time 16 healthy embryos were obtained from the recipient patient, which increases the chances of pregnancy on this second occasion.
Highly complex surgery
Anatomically, the uterus is a very complex organ. It has a network of small, fragile veins instead of visible, well-established veins as occurs in other organs. The vascularization of this organ increases 20-fold when a woman is pregnant, but it is very poorly vascularized when she is not.
“We are talking about what is probably the most complex transplant ever undertaken. Only comparable to face transplants”, explains Dr. Antonio Alcaraz.
This second transplant involved a mother and her daughter, because one of the requirements is that the female candidates must be first- or second-degree relatives. They must meet the immunological compatibility requirements, the donor must already have completed her childbearing, and the two candidates must be healthy. On the one hand, this is to ensure that the surgery does not represent a risk for either of them and, on the other, it is to make sure the recipient tolerates the immunosuppressive treatment well.
“There are very critical moments in the surgery, both in the extraction phase and in the implantation, and part of the complexity comes from this. You need to concentrate intensely for many hours”, says Dr. Antonio Alcaraz.
“It is a marathon in which there are category 1 mountain passes that you have to go through, and it is not over until you reach the end. I would say the most difficult peak is almost at the end of the donor’s surgery when the uterus is only attached by the arteries and veins that we are going to keep. At this point, it is extremely easy to make a mistake, to make a sudden movement that damages the vascularization, which would mean we would lose the organ”, adds Dr. Francisco Carmona.
Currently, approximately 100 transplants have been carried out worldwide, and their viability is around 80%. And 30 babies have been born so far. In general, attempts at embryo transfer start around 6 months after the operation, and women usually get pregnant after the fourth or fifth transfer. With this type of transplant, the viable healthy live birth rate is 40%, whilst with standard IVF, the viable live birth rate per couple starting the process is less than 20%.
What guarantees success
This operation, part of a research project that began five years ago, aims to validate the viability of this surgery with approval to perform 5 transplants in women with Rokitansky syndrome over the course of the project. This syndrome is a disorder involving a congenital defect in the female reproductive system. Women with it are born without a uterus or fallopian tubes. The project involves a team made up of over 50 professionals. Twenty of them carried out the operation, including specialists in urological and gynaecological surgery, anaesthesia and nursing staff. This demonstrates the hospital’s capacity to organize a multidisciplinary team, the coordination of which is an important step in guaranteeing success.
“These are surgeries for very select teams, fewer than 10 teams in the world are able to perform them, which places the hospital among the elite of world surgery”, notes Dr. Francisco Carmona.
Not only is a cohesive team necessary, so are highly specialized surgeons capable of transplanting an organ such as the uterus, which can allow other transplants to be carried out in women who have had this organ removed or who do not have a functional uterus. Performing this transplant at the Hospital Clínic is a technological breakthrough that paves the way for other transplants such as the transplantation of kidneys or of other organs in children with very low birth weight who have blood vessels very similar to those found in the uterus.
“We are making good progress but we have not yet reached the goal. We lack the final success, which is to be able to delivery a baby”, says Dr. Francisco Carmona.
Pictures of the second uterus trasplant