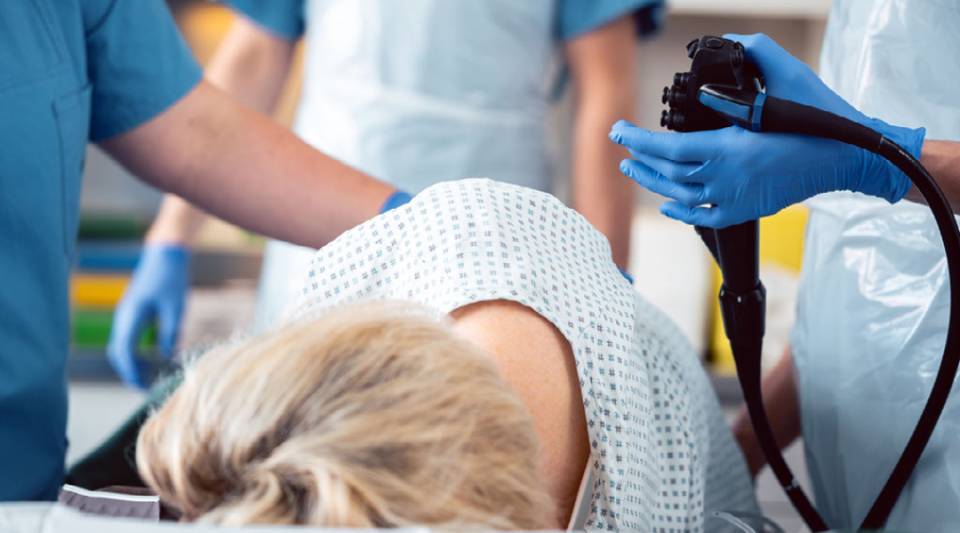
A colonoscopy is a test for the prevention and detection of colorectal cancer but also evaluates symptoms such as bleeding or chronic diarrhoea. It consists of introducing a thin flexible tube about the diameter of a finger through the anus to obtain images of the intestine. The tube, which has a camera and light, is advanced into the colon and images are displayed on a video monitor. Treatments can also be performed through an operating channel through which auxiliary material can be introduced if necessary. The whole procedure from preparation to recovery takes 2-3 hours, but the test itself usually takes less than 45 minutes. It is best to be accompanied before and after the test.
Before a colonoscopy, you need to follow a fibre-free diet and drink fluids to clean out the colon, and you must not eat for 6 hours before the test. During the test, gas (air or CO2) and a rapidly eliminated general anaesthetic are introduced into the colon; no pain is experienced. If any areas with bleeding are seen, drugs are injected through the operating channel and the bleeding is cauterised to seal the blood vessels. Any polyps found are removed and analysed later. After the test, you may feel cramps or swelling due to the air introduced into the colon, which will gradually disappear as the gas is expelled. If a polyp is removed, a special diet must be followed and certain activities are restricted.
Large intestine cancer is the most commonly found in Catalonia, where it is the second highest cause of death from cancer in men and women. For this reason, in 2009, the programme for the early detection of colon and rectal cancer began in Barcelona, coordinated by the Hospital Clínic and the Hospital del Mar, with the idea of diagnosing and treating it as soon as possible and increasing the chances of a cure.
“Every 2 years, everyone from 50-69 years of age receives a letter inviting them to take a test to detect blood in stools that cannot be seen with the naked eye. The person goes to the pharmacy, where they explain how the test is done. Then they go home, do the test and return the sample to the pharmacy. The result (positive or negative) is given over the phone. If positive, a colonoscopy is performed to check for lesions,” explains Dr Francesc Balaguer, head of the Hospital Clínic Gastroenterology Service.
Improvement in the quality of colonoscopies has led to greater early detection of colorectal cancer. This is especially beneficial in higher-risk patients, such as those with Lynch syndrome, the most common form of hereditary colorectal cancer. Patients with this syndrome have a 70% higher risk of developing this type of cancer. A study published last year by Dr Balaguer showed that the quality of the colonoscopy, bowel preparation before the test, the use of high-definition endoscopes and chromoendoscopy (a type of endoscopy that uses dyes or image filters to better visualise lesions) led to better detection of pre-malignant lesions. In addition, performing endoscopies every 2 years helps prevent the disease or to catch it in time.
The Hospital Clínic carries out many colorectal cancer screening studies. For example, a study based on analysing microRNA in tests for blood in faeces was published in 2019. An agreement was signed this November with the Japanese company, Eiken Chemical, to finance the first phase of a study to analyse the efficacy and profitability of the new test. This will be led by Dr Antoni Castells, head of the IDIBAPS Gastrointestinal and Pancreatic Oncology group in the Liver and Digestive Diseases area of CIBER (CIBEREHD), Hospital Clínic medical director and University of Barcelona professor, and Dr Meritxell Gironella, CIBEREHD researcher, attached to the same group.
Recently, the hospital also led a project based on artificial intelligence that improves diagnostic accuracy . And in July of that year, a study led by Dr Sergi Castellví-Bel, head of the IDIBAPS group, Genetic predisposition to gastrointestinal cancer, was published. It was based on the analysis of genetic variants associated with the risk of developing colorectal cancer, to reduce the number of unnecessary colonoscopies.