Researchers from IDIBAPS-Clínic Barcelona have coordinated a study to identify the mechanisms that determine the evolution of leukaemia, relapses following treatment, and its transformation into a very aggressive lymphoma in the final phase for some patients.
The study, published in the journal Nature Medicine and financed with a grant from the CaixaResearch call for health research of one million euros, shows that cells that cause post-treatment relapse and that give rise to the transformation of leukaemia into a very aggressive tumour can already be detected in a very small quantity at the start of the disease, many years before these complications reveal themselves clinically. The results of this work change the view held to date on how leukaemia progresses.
The article has been coordinated by Dr Elías Campo, director of IDIBAPS and head of the Molecular pathology in lymphoid neoplasms group and Dr Ferran Nadeu, post-doctoral researcher at IDIBAPS and the CIBERONC. The first co-authors of the study are, in addition to Ferran Nadeu, Romina Royo, researcher at the Barcelona Supercomputing Center (BSC); Ramon Massoni-Badosa, researcher at the National Centre for Genomic Analysis (CNAG-CRG); Heribert Playa-Albinyana, researcher at IDIBAPS and the CIBERONC; and Beatriz García-Torre, researcher at IDIBAPS.
The Big Bang theory of cancer evolution
Until now it was believed that leukaemia progressed because its cells evolved over the course of time and transformed into more aggressive tumours because they acquired alterations to their genome in a progressive manner that made them more resistant to treatments. This new study shows that some of the leukaemia cells have already acquired these alterations right at the start of the disease, but they are only found in very small quantities. During the evolution of the disease, these more malignant cells will grow and progressively be selected, giving clinical complications many years after disease onset. “It is as if the leukaemia parent cell had engendered numerous daughter cell seeds from the onset of the disease, each of them with different alterations that will enable them to grow in the future when conditions become more suitable”, explains Elías Campo.
These observations confirm the so-called “Big Bang” theory of cancer evolution that proposes that the original malignant cell rapidly multiplies into a large number of very diverse daughter cells with numerous alterations that give rise to future complications through a selection process of those best adapted. “This new view of the disease opens the door to developing highly sensitive diagnostic tests that will enable us to detect and treat these malignant seeds many years before they can grow in an uncontrolled way”, affirms Elías Campo.
The transformation of chronic lymphatic leukaemia into a more aggressive tumour
Chronic lymphatic leukaemia (CLL) is the most frequent leukaemia in the western world, with a frequency of some 5 cases per 100,000 inhabitants per year. It is usually slow-growing, but can evolve towards a very aggressive large B-cell lymphoma that has an average survival rate of below one year. This tumoral transformation occurs in approximately 5-10% of patients.
For the study published in Nature Medicine, the researchers proposed an in-depth study of the alterations that determine the progression of leukaemia taking blood samples obtained at different stages of the disease and using new, highly sensitive techniques that include individual genome sequencing of thousands of tumoral cells at each point in their evolution. They collected samples from tumours from 19 patients with CLL, from the time of their diagnosis to their relapses after different treatments and up to the point of their transformation into an aggressive lymphoma, covering up to 19 years after the start of the disease.
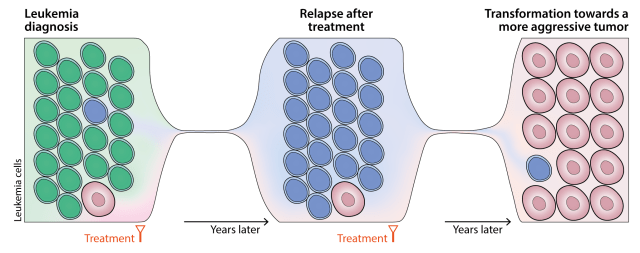
In the study, the genomic alterations were identified that determine the progression and, surprisingly, they saw that a few cells at the earliest point of the disease already had these alterations.
Furthermore, they also identified alterations in the metabolism of these more aggressive cells that, fortunately, seem to be a weakness for them, an Achilles’ heel that could be taken advantage of in order to treat or prevent these complications. “We have seen that if we treat the transformed cells with a drug that blocks this metabolism, we markedly reduce their growth” comments Ferran Nadeu. This drug is already being tested in clinical trials in patients with other types of leukaemia and solid tumours and the current study suggests that it could also be used in chronic lymphatic leukaemia.
“This research illustrates how an aggressive transformation occurs within the context of a slow-growing cancer, a phenomenon that could be explored beyond this type of leukaemia”, notes Elías Campo. “The study shows that single-cell RNA and DNA sequencing is a necessary tool for in-depth analysis of the biology of cancer and it will help us to diagnose and find new treatments for tackling the disease”, he concludes.
The study has been made possible thanks to funding from the Fundació “la Caixa” and the European Research Council (ERC) to Dr Elías Campo and from the American Association for Cancer Research (AACR), the European Haematology Association (EHA) and the Lady Tata Memorial Trust to Dr Ferran Nadeu.
Study reference:
Detection of early seeding of Richter transformation in chronic lymphocytic leukemia.
Nadeu F, Royo R, Massoni-Badosa R, Playa-Albinyana H, Garcia-Torre B, Duran-Ferrer M, Dawson KJ, Kulis M, Diaz-Navarro A, Villamor N, Melero JL, Chapaprieta V, Dueso-Barroso A, Delgado J, Moia R, Ruiz-Gil S, Marchese D, Giró A, Verdaguer-Dot N, Romo M, Clot G, Rozman M, Frigola G, Rivas-Delgado A, Baumann T, Alcoceba M, González M, Climent F, Abrisqueta P, Castellví J, Bosch F, Aymerich M, Enjuanes A, Ruiz-Gaspà S, López-Guillermo A, Jares P, Beà S, Capella-Gutierrez S, Gelpí JL, López-Bigas N, Torrents D, Campbell PJ, Gut I, Rossi D, Gaidano G, Puente XS, Garcia-Roves PM, Colomer D, Heyn H, Maura F, Martín-Subero JI, Campo E.
Nat Med. 2022 Aug;28(8):1662-1671. doi: 10.1038/s41591-022-01927-8.




