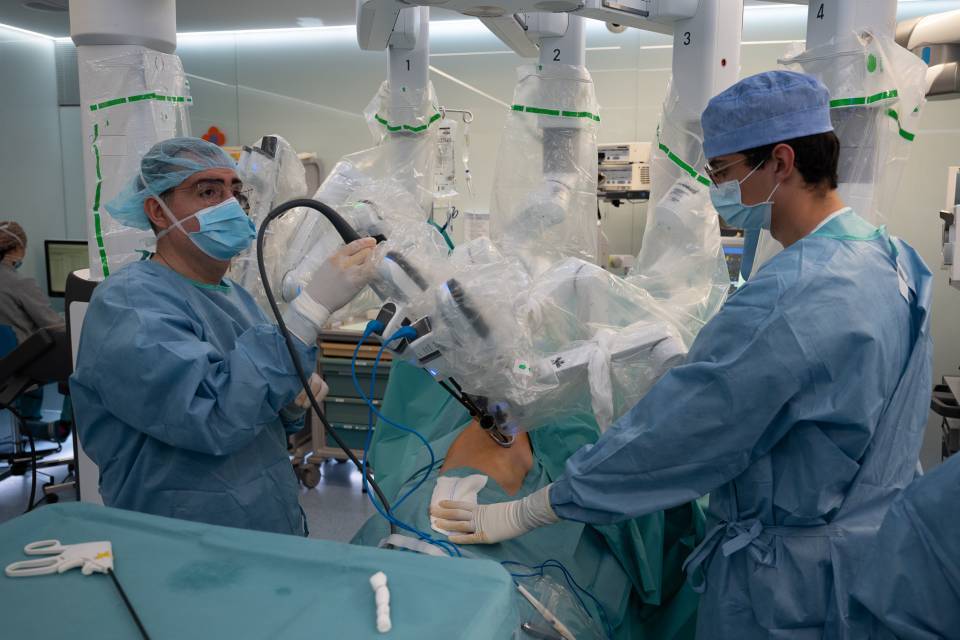
The Hospital Clínic de Barcelona carried out the first pancreas transplant in Spain in 1983, and has remained the top Spanish centre in terms of the number of procedures performed each year since then, with a cumulative total of over 600 transplants. It is currently the Spanish National Health System Referral Centre (CSUR) for simultaneous pancreas-kidney (SPK) transplantation for five autonomous communities and Andorra. Many times it is necessary to transplant the two organs, since the kidney is also affected by the complications of diabetes in the pancreas. The Hospital Clínic has performed a total of 24 pancreas-kidney transplants, since the beginning of the year.
Pancreas transplantation is a treatment option for patients with insulin-dependent diabetes mellitus (especially type 1). Pancreas transplantation involves complex surgery during which the entire pancreas from a deceased donor is transplanted into the patient's abdomen. Since a common complication of diabetes is chronic kidney failure, pancreas transplantation is generally carried out simultaneously with kidney transplantation (89%), or else a pancreas is transplanted into a patient who has already had a kidney transplant (10%). There are also special cases in which an isolated pancreas transplant is performed (1%).
The experience of three transplant patients
Ramon laughs again
Ramon underwent a pancreas-kidney transplant at the Hospital Clínic 7 months ago. He was diagnosed with type 1 diabetes 26 years ago, which led him to be admitted to hospital several times due to severe drops in his blood sugar level. He even lost consciousness on several occasions. His “uncontrolled” diabetes started to affect his kidney and he had to begin to have dialysis sessions every other day. Ramon admits that for him “the worst times were after the dialysis sessions”, and that he only felt well on the days he didn’t have them.
Ramon received a call from the Hospital Clínic at 3 am telling him it might be possible to perform the transplant. The operation went well. “I can walk, eat and laugh again, I had even lost my smile”, he explains, visibly moved.
Maria Josep was determined that her illness would not define her life
Maria Josep is 57, and 23 years ago a Hospital Clínic team performed a pancreas-kidney transplant on her. When she was only 15 she was diagnosed with type 1 diabetes. She remembers that that time “was very hard” and she even had to inject herself 4 times a day. However, Maria Josep wanted to get on with her life and was very clear that her life “was not going to depend on diabetes. I did not want to depend on the disease”.
She explains that at that time, in the late 1990s, mobile phones were just beginning to appear and that, finally, she was given one. “The only numbers I had saved on the phone were my mother's, my sister’s and the Hospital Clínic’s”, she explains. When she received the call asking her to go to hospital for a transplant, she ran straight there without even going home first. Now, 13 years after that operation “I have regained my freedom, and my complications due to diabetes have stabilized or disappeared” she concludes.
Now Laura can start making plans for the future
In September this year, Laura received a pancreas-kidney transplant. Finally, she can start making plans for the future after 17 months of haemodialysis sessions. Laura had to watch what she ate and drank and she barely urinated. "After each dialysis session I was exhausted”, she explains from her bed, where she is still recovering from the operation, but with a smile on her face.
Laura admits that, “when I saw my dad crying because the day of the transplant had arrived, you realize how much your loved ones and those close to you suffer”. Now she no longer thinks about how she will be when she is 50 or 60, “the diabetes problems have gone and I have started a new life. I’m optimistic about the future”, she says excitedly.
A complex procedure that requires a great deal of coordination
The pancreas-kidney transplant is a complex procedure, which requires the participation of different disciplines. According to Dr. Joana Ferrer, a surgeon from the Hospital Clínic General and Digestive Surgery Service, “this type of transplant is the only therapy that has proven to be effective”. Nevertheless, Dr. Ramon Rull, who also works in the General and Digestive Surgery Service, explains that, “we have to assess whether this organ is really the best match for the recipient. It is a very complex technique and at some point we have to decide whether to go ahead with the transplant or not”. Dr. Ferrer concludes that, “the survival of the graft and the patient has improved, and that is due to advances in the immunosuppression protocol, the surgical technique and the pre-operative patient care. Transplantation greatly improves the patient’s quality of life, that is undeniable”.
Other professionals involved in the whole process are endocrinologists and nephrologists. Dr. Antonio Amorfrom the Hospital Clínic Endocrinology and Nutrition Service, is one of those in charge of selecting the ideal candidates for transplantation, and of checking for type 1 or type 2 diabetes, low pancreatic reserve, so that the patients can benefit from this procedure. Dr. Amor also explains that, “we monitor some patients whose pancreatic function is deteriorating, and we work out what the best treatment might be”.
Meanwhile, Dr. Frederic Cofan of the Nephrology and Kidney Transplant Service points out that, “a double transplant, of the kidney and the pancreas, allows the patient to stop taking insulin, there is no need for dialysis, it avoids cardiovascular lesions, their survival rate is higher and it stabilizes eye damage, which can be significant in some diabetic patients”.
Pancreas transplantation
Pancreas transplantation is a treatment option for patients with insulin-dependent diabetes mellitus (especially type 1). Pancreas transplantation involves complex surgery during which the entire pancreas from a deceased donor is transplanted into the patient’s abdomen.
Diabetes mellitus is a chronic disease that is characterized by an increase in sugar (glucose) levels in the blood. In patients with diabetes mellitus, strict blood glucose control is essential to prevent chronic complications such as chronic kidney disease (kidney damage), diabetic retinopathy (eye disease), or diabetic neuropathy (nerve disease).
The main objective of pancreas transplantation is to implant into the recipient cells that produce the exact amount of insulin required at any given moment. Patients with a functioning pancreas transplant are thus able to maintain normal blood glucose levels without needing any other treatment for diabetes. A functioning pancreas graft is able to produce insulin to meet each patient’s metabolic needs, establishing a euglycaemic state, which allows normal glycated haemoglobin (HbA1c) values to be achieved without any critical hypoglycaemic episodes