- Pregnancy
- Symptoms
- Tests and Follow-up
- Healthy habits
- Alarm signs
- Delivery
- Post-partum
- Examinations on the baby
- Breastfeeding
- Sudden death
-
The procedure at Clínic
- Team and structure
Tests and follow-up during Pregnancy
The first monitoring visit is made approximately between weeks 8 and 10. In this visit, the initial weight and height is measured. This is an important visit, since a series of recommendations and advice are given to the pregnant woman. In this visit, the first laboratory test and ultrasound are requested.
- Low and medium risk pregnancies. The pregnancy monitoring visits are made approximately once a month, from the beginning. Weight and blood pressure are monitored in each visit.
- High and very high risk pregnancies. The frequency of the visits may be higher and specific tests are requested for each disease. The doctor indicates the most suitable follow-up in each case.

Blood tests. These are performed between weeks 9 and 10, and are to find out your blood group and Rh factor (e.g.: A+), to detect any possible anaemia (haemoglobin, red cells, etc.), and serology tests (your immune status) against some infectious diseases that could affect the foetus.
The serology tests measured in this first analysis are:
- Toxoplasmosis. It is an infectious disease caused by a protozoon, which, in the case of pregnancy can cross the placental barrier and affect the future baby. It is contagious from contact with cat faeces, eating raw or undercooked meat contaminated with the parasite, as well as raw vegetables. A very high percentage of women have antibodies or defence against the parasite because they have already had it (the majority with no apparent symptoms). The test is performed on the first blood test, and if it is negative it will be repeated with each blood test.
The infection can be prevented in more than 60% of cases with a series of hygiene rules:
-
- Avoid contact with cat faeces.
- Wash the hands with soap before and after handling any foods.
- Try not to touch the eyes, nose, or mouth with dirty hands.
- Toxoplasma dies at 72° C and with freezing at -22° C for 48 hours. Avoid raw or undercooked meat and cured meats like serrano ham that may not have been previously cooked or frozen.
- Peel, or wash with a bleach suitable for foods, the fruit and vegetables that are eaten raw and rinse them well.
- Wash and disinfect the utensils and surfaces that are going to be used in the preparations of the foods and, regularly, the refrigerator.
- Use gloves for garden tasks and handling soil. Wash your hands afterwards.
- Rubella: Also called German measles, is a childhood disease that, if it is contracted during pregnancy, may be a serious threat to the foetus. It forms part of the Triple virus vaccine that was introduce into the Spanish vaccine calendar in 1981. Pregnant women who are not immune must consider receiving the vaccine after delivery, in order to be immunised in any subsequent pregnancies.
- Syphilis and AIDS They are sexually transmitted diseases that are passed to the foetus and may severely affect its development. The detection of the disease in the mother means that she will receive treatment and reduce the risk for both.

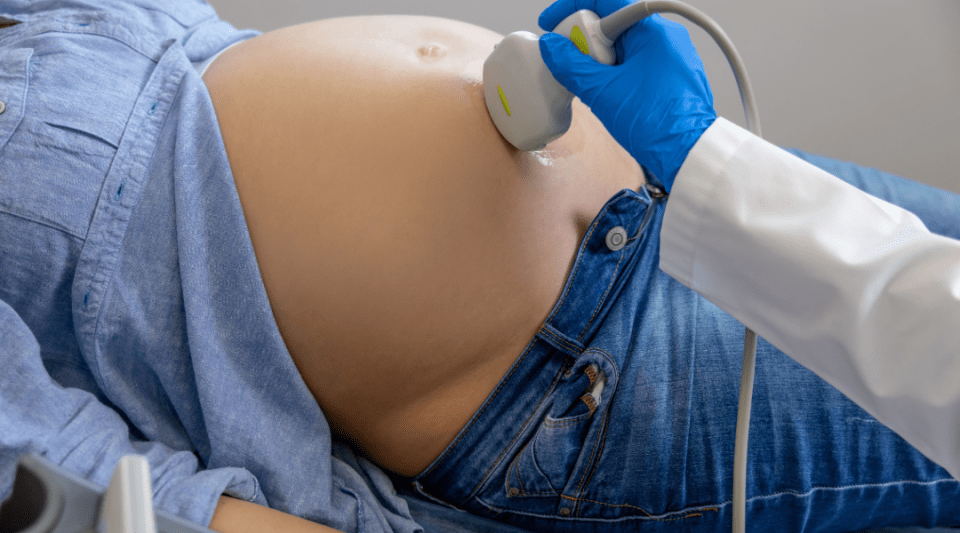
Ultrasound. The first ultrasound is performed between week 12 and 13 of the pregnancy when it is possible to detect any morphological anomalies (shape) early. Using the measurements of the embryo puts a date on the pregnancy and the probable date of delivery can be set. You are given a report and an image of the ultrasound each time it is performed, if you so wish.

Urine culture. This is performed at week 16, even if you have no symptoms, in order to rule out any urine infection that could affect the foetus.

Biochemical screening. It is possible to do this in the first trimester, by combining the laboratory results with the ultrasound examination, and enables making an evaluation of the risk that the foetus has of having Down’s syndrome and Edwards’s syndrome chromosome aberrations. If the result is high risk diagnostic tests are offered: amniocentesis or chorion biopsy, which are invasive prenatal diagnostic tests that can be performed as an outpatient, and provide the complete karyotype of the foetus (chromosome map).

Si el resultat és d'alt risc, es fan les proves diagnòstiques amniocentesi o biòpsia corial, que són proves invasives de diagnòstic prenatal ambulatòries, el resultat de les quals és el cariotip complet del fetus (mapa de cromosomes).

Second trimester morphology ultrasound. It is performed around week 20 of the pregnancy and with it can be observed and evaluated the state of the organs and structures of the foetus. The placenta and the amount of amniotic fluid are also assessed. It is an important ultrasound because the majority of the organs are now formed. If a defect is detected in any of the organs, more specific ultrasounds can be requested. An echocardiogram - a specific ultrasound of the heart, or a neuro-ultrasound – a specific ultrasound of the skull structures, may also be requested in the hospital.

Blood tests. Performed about week 25. As well as other results, details are obtained on hepatitis B, a disease of sexual transmission or blood contact. In case it is present in the maternal blood, after delivery, the baby will be administered a vaccine and gamma-globulin before discharged to home. Fasting is not required for this.

O’ Sullivan Test. It is a test that is used to see how the body reacts to sugar. It consists of drinking a sweet drink and after one hour blood is taken. During this hour you have to remain seated, without smoking or eating anything, since they can change the results. If the result is abnormal, the following step is the Oral Glucose Tolerance Test, a test that is scheduled for another day.

Glucose Tolerance Curve. You will remain in the hospital for about four hours. Special preparation is needed to perform this test. It consists of a diet rich in carbohydrates, the three previous days. On the day of the test, you have to arrive fasting; a first blood sample is taken and, next, a concentrated sweet drink is taken. After, three more blood samples are taken, with one hour difference between each. There are 4 specimens taken in total. Thus, you will remain in the hospital for almost four hours, therefore it is recommended to bring a book or magazine to pass the time.
While the test is being performed you must be seated, without smoking or eating anything, since these may affect the values of the tests. The results will be given by the doctor in the following visit.

Anti-D Gamma-globulin. If the blood group is negative, anti-D Gamma-globulin is administered around week 28 of the pregnancy. The blood group of the baby will be checked at birth and, if positive, you will receive another dose of anti-D Gamma-globulin before hospital discharge.

Blood tests. They are performed around week 32 of the pregnancy and an assessment is made, among other things, on the state of coagulation, which is important during delivery.

Ultrasound. It is performed around week 34 of gestation and is useful to assess foetal growth, the amount of liquid, and the position of the baby.

External version. A procedure that consists of changing the position of the baby by external manual manipulations to place it in the cephalic position. It is performed in week 36 of the pregnancy for those babies that are in the podalic or other positions, with the aim of avoiding an elective caesarean section. Vaginal breech deliveries are not currently performed. The procedure is done as an outpatient, with an ultrasound that guides the whole procedure, and with a cardiotocography recording to monitor the well-being of the foetus at all times. Medication is administered to help in the relaxation of the uterus during the procedure. Fasting is not required for this procedure.

Vaginal and rectal culture. It is performed around week 36 in order to detect Streptococcus agalactiae, which is a microorganism that, if present in the delivery canal, can affect the health of the baby, since it is acquired at birth. To avoid this, an antibiotic can be administered to the mother the same day as the delivery. If the result is negative (the microorganism is not present), the test is repeated in 4 weeks, if the baby has still not been born.
At the end of gestation, the following may be performed:
Vaginal examination. It can be performed in the 40 weeks gestation visit, although it may be performed in any previous visit if there is a determined indication such as, for example, suspicion of amniotic sac rupture.
Cardiotocography recording. Known colloquially as “straps/leashes”, it is performed about week 40, and consists of placing a belt around the abdomen for about 20 minutes, with sensors connected to a monitor or screen. The device records the foetal heartbeat, and contractions if there are any. It is repeated at 41 weeks, and subsequently every 48-72 hours until the time of delivery.
Non-invasive prenatal test (fetal DNA in maternal blood). It is a blood test of the mother that can be performed from 10 weeks of gestation to rule out any chromosome diseases such as Down’s syndrome or Edwards’s syndrome.
The basic difference with the invasive tests (amniocentesis or chorion biopsy) is to do with the risk, since, in invasive tests, there is a small risk of miscarriage, while there is no risk with the blood test. The final result is also different, since in the case of the invasive tests the complete gene map -all the chromosomes- is obtained while with the Harmony Test only the trisomies in four of the chromosomes can be detected.
3D and 4D Ultrasound. A 3D ultrasound is an image of the fixed fetus and with volume, that is, in three dimensions (3D) and an ultrasound in 4D is a 3D ultrasound with movement, that is, a 3D ultrasound in real time.
Substantiated information by:



Published: 20 February 2018
Updated: 26 March 2025
Subscribe
Receive the latest updates related to this content.
(*) Mandatory fields
Thank you for subscribing!
If this is the first time you subscribe you will receive a confirmation email, check your inbox