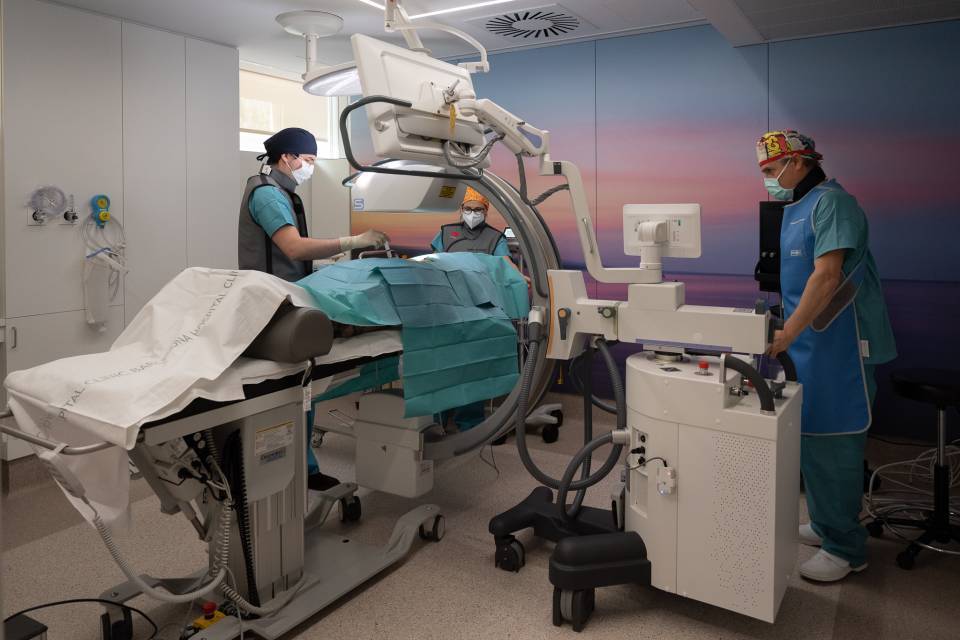
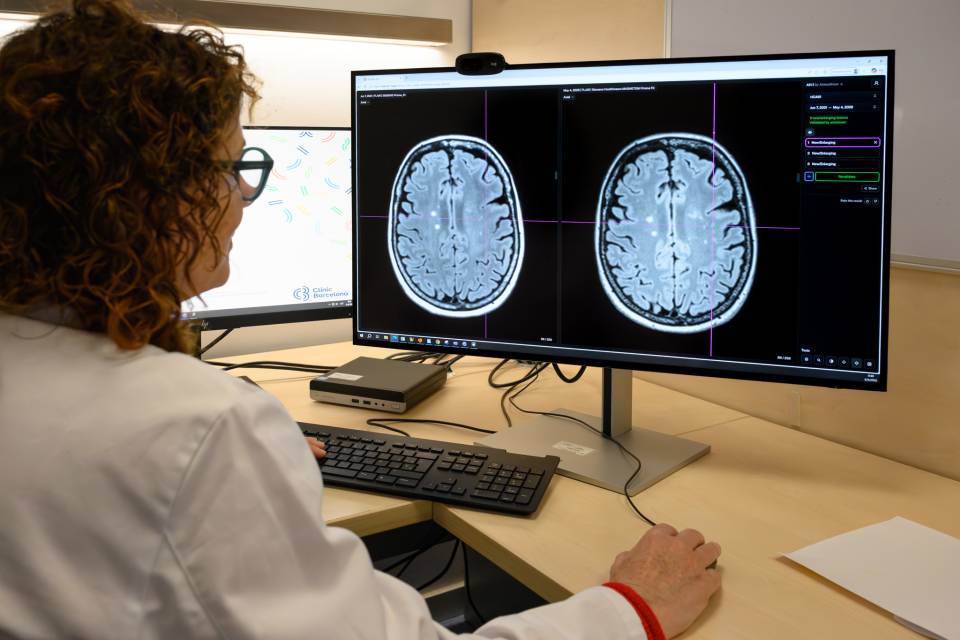
With the opening of this new space, a new way of interacting with patients based on conversation and greater proximity has also been introduced. Last year, the Hospital Clínic Pain Unit, led by Dr. Christian Dürsteler, carried out 9,171 visits (1,334 initial visits and 7,837 subsequent visits) and 3,500 procedures/interventions were performed. Various studies show that 20-30% of the population suffers chronic pain. Pain is a warning mechanism that helps human beings to survive. Under normal circumstances, it warns the body that it is suffering some kind of injury or illness. However, there are situations in which pain does not end when its cause is resolved. It persists over time and can affect different areas of our life, whether emotional, family or work-related.
The new Hospital Clínic Pain Unit involves a paradigm shift in the relationship between patient and professional, since the design of the space facilitates and promotes more two-way communication to favour a more solid and trusting relationship between the two actors, adding the figure of the caregiver as another actor in the therapeutic team. This new way of relating involves moving from consultation to conversation. The new design of the space, built using sustainable materials, was achieved thanks to the co-creation of the space and taking into account the needs of patients and professionals. In short, the new space of the Pain Unit is warmer, since the treatments are carried out in a friendlier and more comfortable space.
https://www.youtube.com/watch?v=AL0sUkBOsx4
With the launch of this new space at the Hospital Clínic, we also want to promote the new “first conversation” protocol between patients and professionals, which has three phases. Firstly, there is a questionnaire that the patients can fill in at home, which helps them to prepare the visit. Secondly, there is a new format for the collection of information by the professional during the consultation/conversation that will facilitate the final diagnosis. And finally, a reminder document with information capsules and resources for the patient to consult after their stay in hospital. With this new methodology and this new space, the aim is to create a new way of interacting with the patients in which they can better manage their expectations.
The Pain Clinic at the Hospital Clínic Barcelona is made up of 22 professionals, including anaesthesiologists specializing in the treatment of complex pain. It treats patients with chronic pain due to cancer, neuropathic pain, and pain after back surgery, who are referred by primary care specialists from the primary healthcare centres (CAPs) (AISBE Barcelona Esquerra de l’Eixample) or from the hospital itself. Exceptionally, patients from other healthcare areas are accepted, depending on the patient’s illness (e.g. patients who have undergone transplants at the hospital, patients with rare diseases, etc.). Along with a specialized nursing team, postoperative monitoring is carried out in the hospital wards of patients who have undergone particularly painful surgical procedures. This new space also involves professionals from family medicine, rehabilitation, oncology, neurosurgery, and advanced practice nursing.
According to Dr. Christian Dürsteler, head of the Pain Section in the Hospital Clínic Anaesthesiology Service, “chronic pain is, in part, an emotion. With this new space, we want to help the patient throughout their process, make them participate in their decisions, and offer them personalized treatment in a comfortable environment”. Moreover, Dr. Dürsteler stresses that, “the biopsychosocial approach to pain has been promoted, in which patients are not only treated with drugs and/or interventions, but all the dimensions of the person are affected. In this context, the PAINDOC (Comprehensive Care for Patients with Chronic Pain) Programme was created. It consists of 8 group sessions (therapeutic education, psychological support, mindfulness meditation and guided physical exercise)”. “This programme provides pain management tools that are easy to incorporate into the daily lives of patients and caregivers, promoting the empowerment and self-management of the disease”, he concludes.
This initiative was promoted by the Strategy and Planning Management as an innovation project scalable to other hospital services, with the participation of AheadPSP architects, the Infrastructures and Biomedical Engineering Management, The Care Lab (an external consultancy firm specializing in Design Thinking), and the patient participation programme promoted by Dr. Joan Escarrabill and the Patient Experience Forum team.