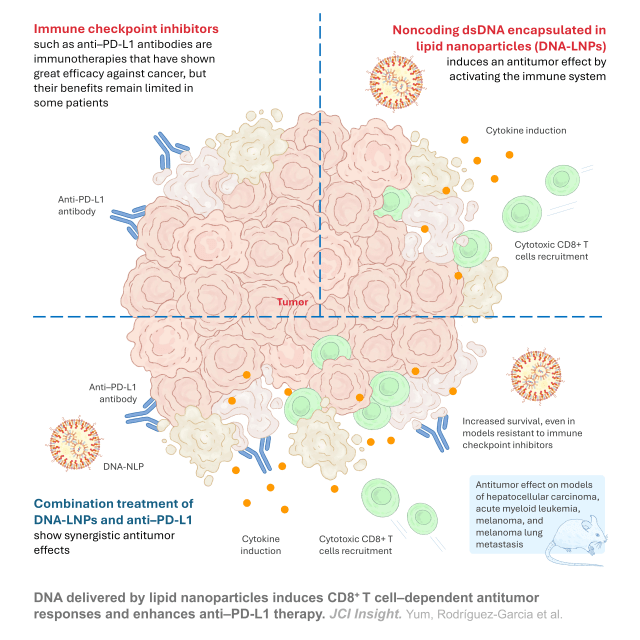
Immune checkpoint inhibitors have revolutionised the treatment of a range of cancers, as they prevent the immunosuppressive effect of tumours and allow the cells of the immune system of patients to attack the cancer. Even so, a large proportion of patients do not respond, or experience relapses, mainly because their tumours have little previous immune activity. For this reason, one of the great challenges in immunotherapy is to find ways of “activating” the immune system and thus convert cold tumours with low immune activity) into “warm” tumours, where these drugs are much more effective.
Based on this need, the Clínic-IDIBAPS team, working within the Clínic Barcelona Comprehensive Cancer Centre, investigated whether administering non-coding DNA encapsulated in lipid nanoparticles could strengthen the patient’s own anti-tumour immune response.
"Our hypothesis was simple: if we can manage to turn on the innate alarm mechanisms of the immune system within the tumour, we can make it easier for treatment with immune checkpoint inhibitors to work in many more cases," explains Guedan.
Results in various tumour models
The experiments have been carried out in mouse models of hepatocellular carcinoma, acute myeloid leukaemia and melanoma. In all of them, the administration of nanoparticles caused: a strong immune activation, with increased cytokines and recruitment of cytotoxic lymphocytes to the tumour; a decrease in tumour growth; and a significant prolongation of the animals’ survival.
One of the most relevant results is that nanoparticles show a synergic effect with the immune control points inhibitor, notably expanding survival both in sensitive tumours and in tumours resistant to such treatments. This synergy does not increase the adverse effects and, in some cases, permits reduction in the necessary dose of nanoparticles without losing efficacy.
According to Alba Rodríguez‑Garcia, one of the first-named authors of the study and researcher in the cellular immunotherapies for cancer, “our results indicate that this strategy has potential to increase the number of patients that benefit from this immunotherapy. It is especially promising to see that it also functions in resistant models, one of the great clinical challenges of today.”
Towards new immunotherapy combinations
Activating the immune system within a tumour could become a key tool to ensure that patients respond to immunotherapy. Furthermore, the nanoparticles Technology will permit in future incorporate other immunomodulatory molecules or adapt them to direct them at other types of specific tumours.
The group expects to continue the preclinical studies to determine what tumours could benefit further and explore options to translate this strategy to initial clinical trials.
The study was conducted in collaboration with Spark Therapeutics, the Roche Group company, which has developed the nanoparticles and has contributed to the characterisation in other tumoral models, while the experimental part in hepatocellular carcinoma has been carried out entirely at IDIBAPS.
Study of reference
DNA delivered by lipid nanoparticles induces CD8+ T cell–dependent antitumor responses and enhances anti–PD-L1 therapy. Seoyun Yum et al. JCI Insights. March 23, 2026