- What is it?
- Causes and risk factors
- Symptoms
- Diagnosis
- Treatment
- Progression
- Living with the disease
- Research lines
- Frequently asked questions
What is Multiple Sclerosis?
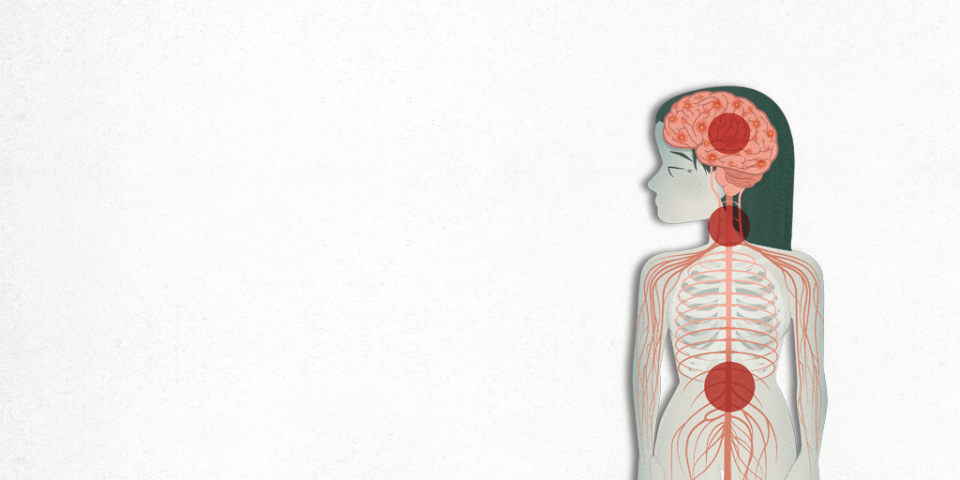
Multiple sclerosis is a chronic neurological disease that affects the central nervous system, that is, the brain and the spinal cord. The symptoms vary from patient to patient and each one develops individually depending on the area that is damaged. Multiple sclerosis is the second cause, after traumas, of neurological disability among young adults and affects more women than men.
Multiple Sclerosis explained in first person
People with multiple sclerosis should understand that it is very important to continue then treatment even they don’t have any symptoms, because these medicines don’t treat the symptoms - they help prevent new attacks.
The experience, the years of research mean that we are learning more about it all the time, there are more treatments to manage it, so while it can’t be cured yet, we patients can still have as normal a life as possible.
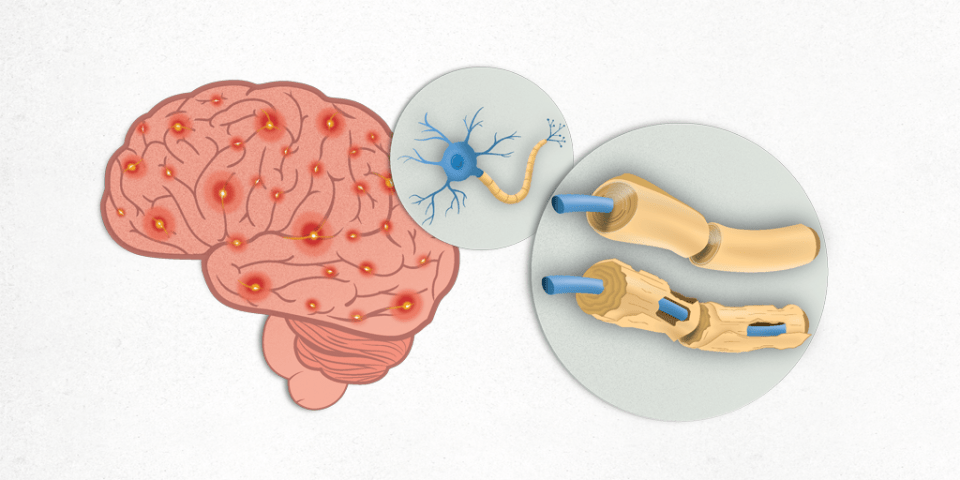
Multiple sclerosis's main features are the appearance of lesions over the nerve fibres and their protective layer, the myelin sheath, a substance consisting of proteins and fats, which helps in the transmission of nerve impulses.
The immune system, which normally protects us from diseases, reacts incorrectly against myelin in many areas, occasionally leaving scars (sclerosis). These scarred areas (lesions) are also known by the name of demyelinating plaques.
These lesions are produced at different times, and in multiple locations in the brain and spinal cord. The symptoms and signs of the disease vary from one person to another depending on the areas affected. Although different people share the same diagnosis, the disease and its progression may be different in each case.
The central nervous system (CNS) is composed of the encephalon and the spinal cord. The encephalon is made up of the brain, the cerebellum and the brain stem. The peripheral nervous system (PNS) comprises the different peripheral nerves that emerge or arrive at the spinal cord and are distributed all over the body.
In the central nervous system two classes of substances can be distinguished due to their colour: the grey matter and the white matter. The grey matter is made up of neuronal bodies, while the white matter corresponds to the neuronal extensions called nerve fibres.
The basic functional unit of the nervous system is the neuron. The neurons generate electrical signals that enable them to rapidly transmit information throughout the body. A neuron consists of a cell body, one or several short extensions (dendrites), and a long extension (axon). The sheath or covering of the axons is myelin. The axons conduct the nerve impulses, and the myelin acts as an insulator and increases the conduction velocity of the nerve impulse.
The neurons are essential for the transmission of impulses, but they cannot fulfil this function without the support of the glial cells. These cells perform very different tasks, such as the supply of nutrients, the maintenance of the structure, or the acceleration of the neuronal conduction itself. The oligodendrocytes are a type of glial cell, which are exclusively located in the encephalon and the spinal cord. These cells create myelin sheaths around the neuronal axons, isolating them and increasing the transmission speed of the electrochemical impulses that travel along them.
Types of multiple sclerosis
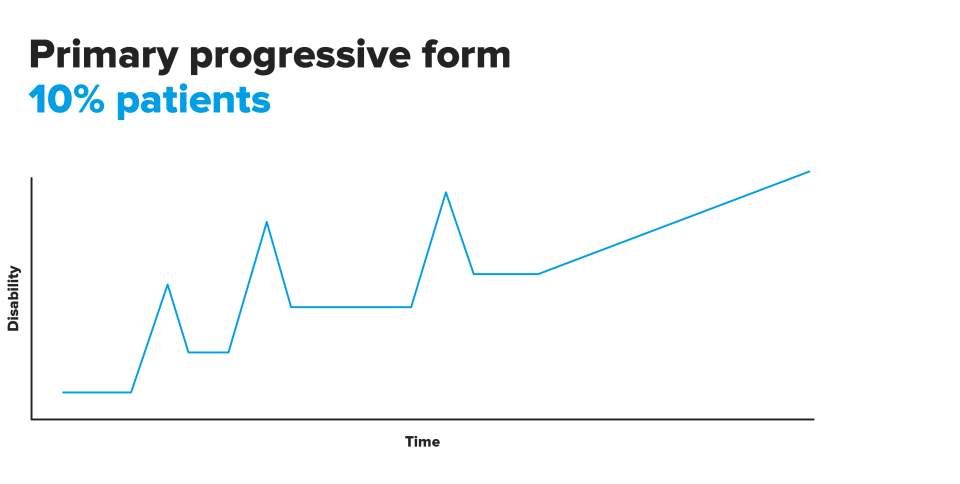
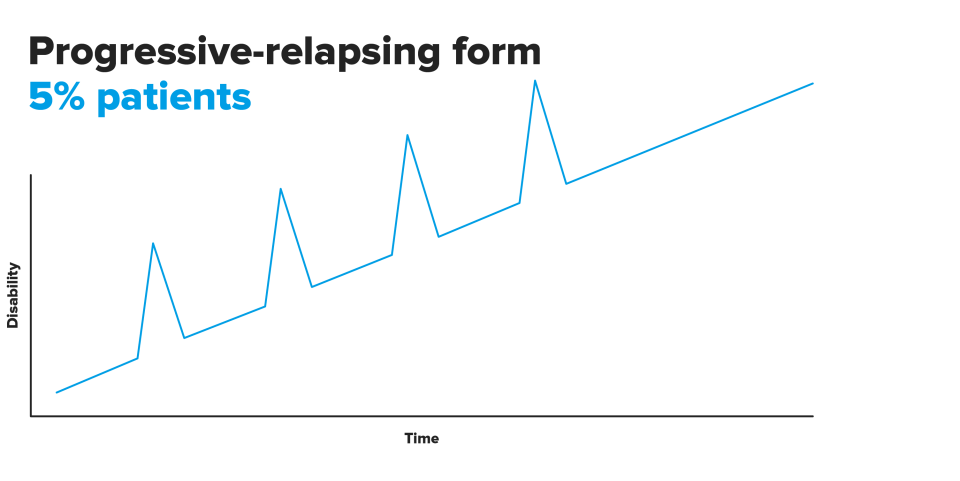
Multiple sclerosis is characterised by the appearance of episodes or flare-ups of neurological dysfunction that remains constant for 3-4 weeks and that are slowly recovered throughout the following month. It must always be a manifestation that does not coincide with a fever or any other state that could alter the general status.
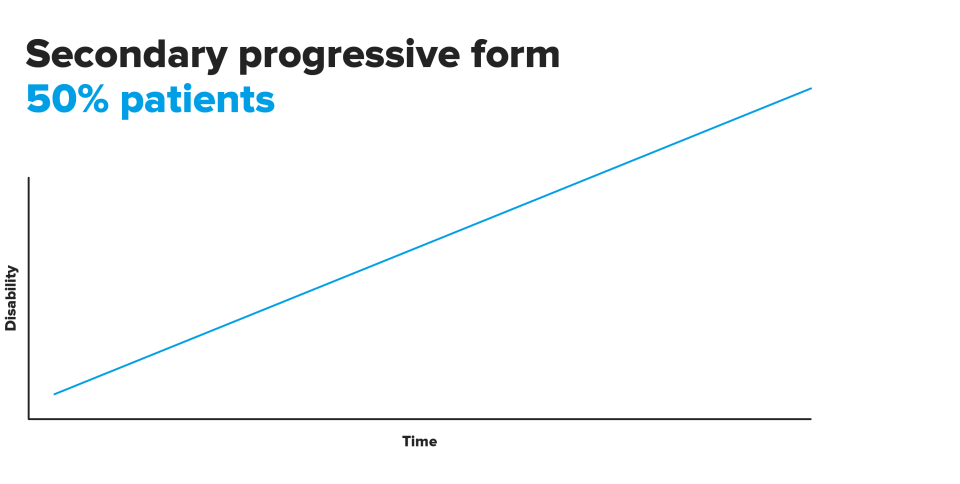
These flare-ups do not always occur in the same way or with the same intensity, and may follow a different course. Based on these differences it may be considered that there are different sub-types of the disease.
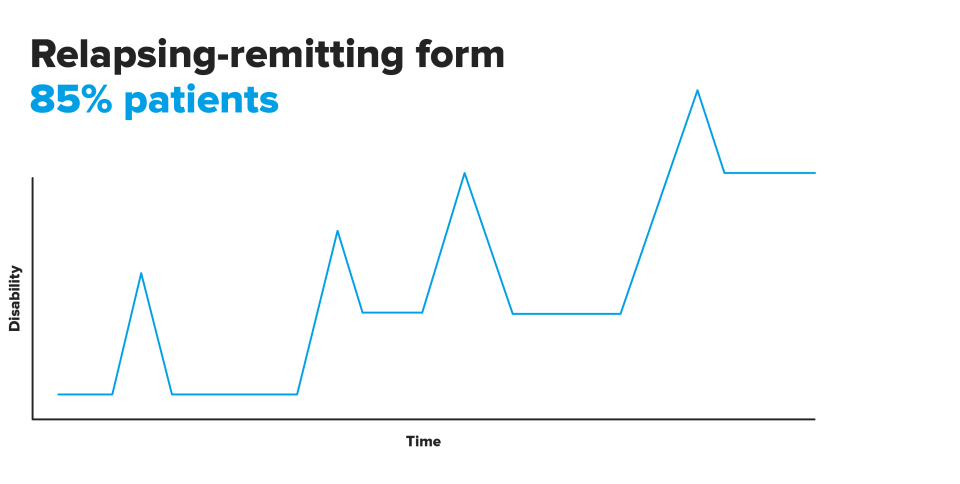
Relapsing-remitting form. It is the most common form, with 8-9 of every 10 patients with multiple sclerosis having this progressive form. It is characterised by the appearance of episodes or flare-ups of neurological dysfunction from which the patient recovers completely or partially (thus the name remitting) and which are repeated every determined time (relapsing).
For these patients that present with the disease in the first episode or flare-up, it is said that they suffer from a clinically isolated syndrome (CIS), which may not necessarily be a multiple sclerosis diagnosis.
How many people are affected by multiple sclerosis?
It is calculated that there are around 2.5 million people affected in the world. In the West, it is the most common chronic neurological disease in young adults. The frequency depends on the geographic location and genetic factors. Thus, it is more common between latitudes 40o and 60o north and south.
In Europe, the number of cases in the northern countries and the United Kingdom is around 2 for every 1,000 inhabitants, which is similar to that of the United States and Canada. In Spain, it is around 1 for every 1,000 inhabitants, which means that about 47,000 people are affected in our country. In Africa, Asia and South America, the disease is less common.
Multiple sclerosis can appear at any age, but it is rare before 10 years, and after 60 years. The average age of onset is at 30 years, with a first peak between 21 and 25 years, and another much lower one between 41 and 45 years. It affects females more than males, in a ratio of 2-3 to 1. In older age groups (over 45 years), the ratio is 1:1.
Substantiated information by:


Published: 20 February 2018
Updated: 20 February 2018
Subscribe
Receive the latest updates related to this content.
Thank you for subscribing!
If this is the first time you subscribe you will receive a confirmation email, check your inbox