- What is it?
- Causes and risk factors
- Signs and symptoms
- Diagnosis
- Treatment
- Evolution of the disease
- Living with the disease
- Research
- Frequently asked questions
-
La enfermedad en el Clínic
-
Equipo y estructura
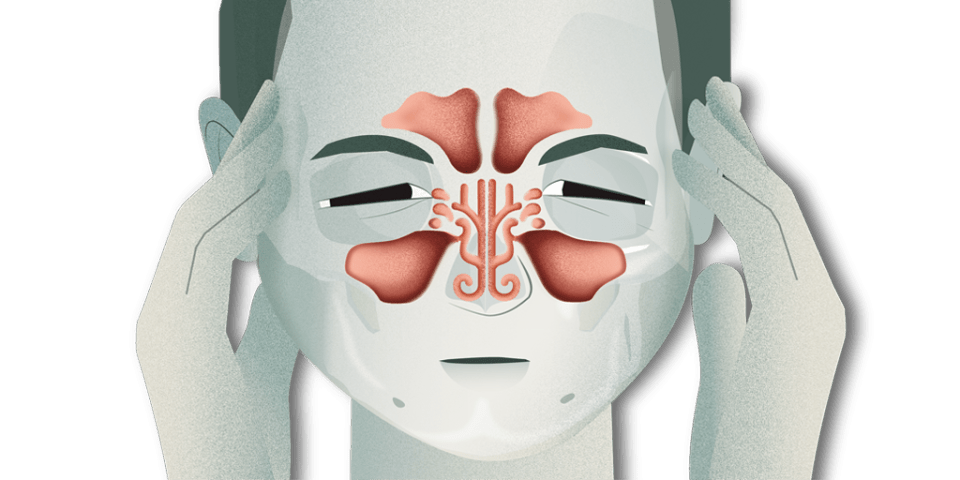
What is rhinosinusitis?
Rhinosinusitis is a very common condition that involves inflammation of the nose and the paranasal sinuses. The paranasal sinuses are cavities located below, above, and around the eyes, inside the nose, and they communicate with each other and with the nasal passages. Under healthy conditions, they are filled with air, but when inflammation of the mucous membranes occurs, they can become blocked, accumulate mucus, and cause inflammation and/or infection that needs to be treated.
Rhinosinusitis explained in first person
The key point in these chronic diseases is maintaining the treatment and strictly adhering to the therapeutic guidelines indicated by the treating doctor. This will ensure the patient remains stable and does not suffer any acute flare-ups which are very hard to treat. Keeping the inflammation under control means the patient will be well managed and have a good quality of life.
First that you'd to do the treatment indicated by the specialist, but then if you have to undergo intervention, do it. Because it totally changes how you face your quality of life.
Sinusitis or rhinosinusitis is defined as symptomatic inflammation of the paranasal sinuses and nasal cavity. Nowadays the term rhinosinusitis has replaced the term sinusitis, as most patients often have symptoms of both rhinitis and sinusitis simultaneously.
Rhinosinusitis is an inflammation of the nasal cavities and the paranasal sinuses characterised by obstruction and/or nasal congestion or alternatively by nasal discharge or a runny nose which may drain at the front or back of the nose. These symptoms can be accompanied by facial pain or pressure and a partial (hyposmia) or total (anosmia) loss of the sense of smell.
A physical examination can reveal nasal polyps and/or mucopurulent discharge or a mucus blockage in the middle orifice (meatus).
Classification of Rhinosinusitis
Rhinosinusitis is classified according to its duration:
Acute. Symptoms lasting less than 12 weeks and which disappear completely. The origin may be viral (including COVID) or bacterial.
Chronic. Symptoms for longer than 12 weeks, they do not disappear and may occasionally worsen (flare-ups). These cases are divided into chronic rhinosinusitis with or without nasal polyps.
Nasal polyps
Nasal polyps are small benign masses caused by an inflammatory process of the sinus mucosa, although their cause is unknown. They can lead to very bothersome symptoms such as loss of smell, inability to breathe through the nose, excessive mucus production, facial pressure, and even nasal deformities.
How many people are affected by Rhinosinusitis?
Acute viral rhinosinusitis (the common cold) is very common. Adults experience an average of 2 to 5 episodes per year, while school-aged children have between 7 and 10. Only 0.5%–2% of acute viral rhinosinusitis cases become secondarily infected with bacteria.
In bacterial rhinosinusitis, symptoms worsen after 5 days or persist beyond 10 days. It occurs in 1 out of every 7 cases, with an incidence in Europe of 10–15%. Rhinosinusitis is an important health problem that represents a significant economic burden on society.
The incidence of chronic rhinosinusitis, with or without polyps, is estimated to be between 5–11% of the total European population. However, the prevalence of chronic rhinosinusitis diagnosed by a specialist is only 1–2%, suggesting that this condition is often overdiagnosed. There are no clear data indicating differences in incidence according to sex. Other studies show that prevalence increases with age, with an average of 2.7% in patients aged 20–29 years and 6.6% in those aged 50–59 years. After age 60, prevalence stabilizes at around 4.7%.
Substantiated information by:

Published: 19 September 2018
Updated: 21 October 2025
Subscribe
Receive the latest updates related to this content.
(*) Mandatory fields
Thank you for subscribing!
If this is the first time you subscribe you will receive a confirmation email, check your inbox