- What is it?
- Symptoms
- Causes
- Tests and diagnosis
- Treatment
- Disease evolution
- Living with disease
- Research lines
- Frequently Asked Questions
- Prevention
-
La enfermedad en el Clínic
-
Equipo y estructura
Treatment of Chronic Obstructive Pulmonary Disease
The cornerstone of COPD treatment is giving up smoking and taking up general healthy habits, such as a balanced diet and regular physical exercise. It is also important to avoid environments that can cause irritation of the airways, like smoking areas, particularly in passive smoker situations, contamination, low temperatures, etc.
Stopping smoking is probably the best decision you can make. Although it is difficult, it is not impossible and has many beneficial effects. Go to your Primary Care Centre, since there are many health professionals that will be able to help you to quit this habit and it will be easier to achieve it.
Where to start
- Why do I smoke? Ask yourself why you smoke every time you light up a cigarette, and remember that smoking is the first cause of avoidable death in the developed countries.
- Look for motivation. Write a list with the reasons, think again about how much and when you smoke and make a daily record sheet: day, time, place / activity, reason.
- Avoid situations that are associated with smoking.
- Time of making the decision to stop smoking. Go over the list of reasons for stopping smoking; think of a date within the next four weeks; try not to choose a conflictive date, and fix a day for stopping.
- Tell everyone in your closest circle. Once the decision is made, tell your family, friends, work colleagues.
- Calculate what you are saving. It is advisable to calculate the money that you spend on smoking; think about what you will be able to do with what you save.
- Support. Look for support from a relative or friend who smokes, to try to stop at the same time.
- Avoid the temptation. Remove everything associated with tobacco: ash trays, lighters, cigarettes.
What must I do?
- Get up in the morning a little earlier than usual, do some physical exercises and drink plenty of water and fruit juices. You have to try to be active all day and make the decision not to smoke each day.
The perseverance of not smoking
- Practice any physical activity. It is advisable to have a diet rich in fruit and vegetables. Try not to drink, for now, drinks that are usually accompanied by tobacco, such as coffee, for example.
- If the desire to smoke is very strong. You must not worry. You have to relax, breathe deeply, concentrate on what you are doing, and remember that the desire to smoke only lasts 2 minutes and then its disappears.
- Replacements. There are chewing gums, patches or drugs that can help, but you should remember that to achieve success the most important is the personal commitment. In any event, if you need help you can always consult the health professionals.
- Do not give in not for a single cigarette. The desire to smoke decreases after the second or third week.
- Congratulate yourself every day that you pass without smoking.
The main aims of COPD treatment are summarised in:
- reducing the chronic symptoms of the disease;
- decreasing the frequency and severity of exacerbations;
- improving the prognosis.
The short-term benefits (control of the disease), as well as the medium and long-term ones (reduction in the risk of exacerbations, the accelerated drop in lung function or death) must be achieved.
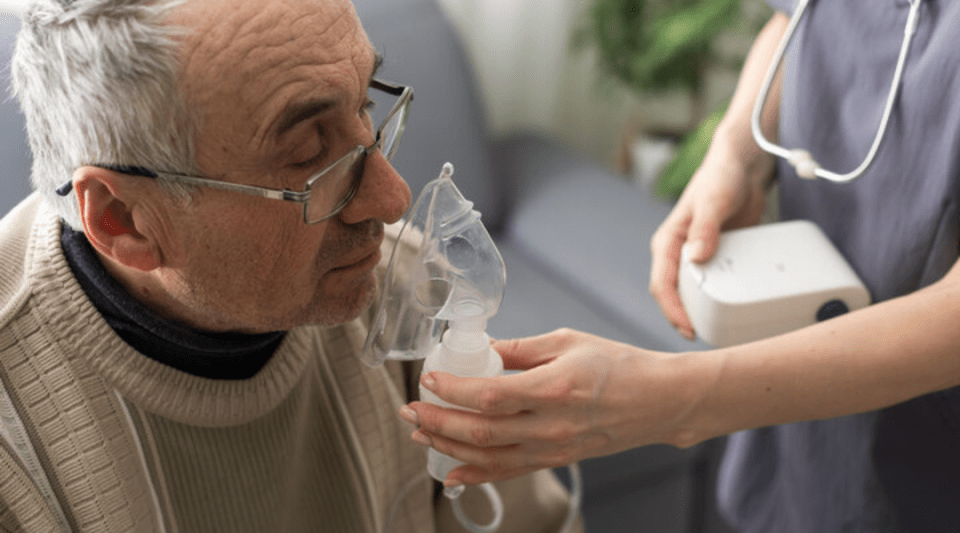
The administration of drugs by inhalation is increasing. The possibility of using drugs in very small doses and make them reach the respiratory system (target organ), the place where they are going to develop their action, provide tranquillity to the patient and the prescribing physician. The positive effects are rapid and effective and have few undesirable effects.
There are many commercial devices used for the administration of the drug, which leads to a more personalised care when proposing a device that better adapts to the needs of the patient, together with proper instruction on the technique. Furthermore, each inhalation device may contain one or several drugs within it. The duration of the dose of each drug is different. Therefore, to know the different inhalation systems and the different possibilities of the drugs available, are important aspects to take into account.
- Bronchodilators. Increase the diameter of bronchi when these have narrowed. The short-acting ones are taken every four or six hours, and the prolonged action ones, every twelve hours.
- Anticholinergics. Act like the bronchodilators: Short-acting (every 4 or 6 hours) and Long-acting (every 24 hours)
- Anti-inflammatory drugs.
- Corticosteroids. Reduce inflammation of the bronchial mucosa. The effect of these medications is noted after several days and last for 12 hours.
In the case of chronic respiratory diseases it is important to take the prescribed medication. Avoid self-medication and stopping the treatment. Do not increase or decrease the doses. The medical team will instruct you when you must take them.
One important aspect is taking the medication every day and done it correctly. Many patients believe that, as they have used sprays for many years they already know how to use them. But this is not the case. Only a small group of patients know how to correctly perform the inhaler technique.
Bullectomy, lung volume reduction, and lung transplant are the three surgical interventions that may be performed in very select patients with COPD. These treatments may lead to improvement in some cases, including functional capacity and quality of life.

Bullectomy. It is a surgical procedure indicated for years for bullous emphysema. One of the consequences of COPD is “air trapping”. The difficulties in the movement of air during the exhalation phase causes the lung not to empty properly and leaves the remains of air that, under normal conditions, would be exhaled. This air is “trapped”. “Air trapping” is usually diffuse. However, in some cases this trapping is irregular and in some areas it is greater than in others. This phenomenon explains the bullae (or “bubbles” of trapped air).
In extreme cases, a type of valve system is produced in some bullae that allows air to enter with inhalation, but not escape during exhaling. These bullae can become very large.
Currently, there is evidence that shows that bullectomy can be beneficial in patients with severe COPD and giant bullae. Resecting a giant bulla decompresses the adjacent lung parenchyma and helps reduce the breathlessness and shortness of breath (dyspnoea) and improve lung function.

Lung volume reduction surgery. Once the medical treatment is optimised, lung volume reduction surgery may be a treatment option in selected patients with COPD and a predominance of emphysema. The best candidates for volume reduction surgery are those with emphysema mainly in the upper lobes and with a low exercise capacity. The results of a large study of over more than 1200 patients with severe emphysema showed volume reduction surgery had a significant although temporary effect on the level of the symptoms or the worsening of the quality of life, which indicates that it mainly has a palliative role.

Lung transplant. Lung transplant has been performed for more than 30 years in patients with end-stage COPD. COPD is the main indication for lung transplant. But although this intervention has shown to have a clear positive impact on lung function in patients with COPD, exercise capacity and quality of life, the benefit in terms of increase in survival is uncertain. However, indirect and convincing evidence shows that when appropriate patient selection criteria for transplant are applied, the quality of life, as well as the survival, improves after transplant.
Lung transplant may be indicated in patients less than 65 years-old and with advanced COPD. The criteria that the lung transplant patient candidate must meet, according to International Guidelines are a BODE (Body-mass index, airflow Obstruction, Dyspnoea, and Exercise) index from 7 to 10, or any of the following: history of hospital admissions due to decompensations and acute respiratory failure, pulmonary hypertension, and low lung capacity.

Home Oxygen. There is scientific evidence that demonstrates that the administration of oxygen more than 15 hours a day improves survival of patients with COPD who have chronic respiratory failure (with low values of oxygen in arterial blood -PaO2-).

Rehabilitation. Regular physical activity is one of the pillars of COPD treatment. The patient with COPD must change their habits and avoid sedentarism. There are studies that show that rehabilitation programs that include multiple elements (exercise training, therapeutic education, etc.) and multidisciplinary interventions improve the symptoms and the quality of life, and have an impact on hospital admissions.
There are no studies that show how to scale these programs so that they could be extended to whole COPD patient population. On the other hand, the patients that have done the training start losing the benefits obtained over time, leading to a need to take part in booster programs.
Rehabilitation programs are very important for selected patient groups, such as candidates for lung transplant, or relatively young patients with a poor response to treatment. In some cases, home rehabilitation programmes have been established.
Home oxygen is a treatment that is administered always using the arterial blood gases results when the patient is in a clinically stable condition. The blood specimen is taken when the patient breathes room air (at least 30 minutes after having stopped taking the oxygen).
The current recommendations for the indication of continuous home oxygen therapy in the stable phase of COPD are: patients that have an arterial blood oxygen level (PaO2) less than 55 mmHg or between 55 and 60 mmHg, if they have an increase in red blood cell volume (polycythaemia), heart disease or heart failure. In any case, all patients with COPD must receive oxygen for a minimum of 15 hours/day (including sleeping hours). The doctor who prescribes the oxygen therapy indicates the amount required, measured in litres per minute (L/m) and the time that it should be used. The most usual oxygen flows that are used vary between 1-3 litres/minute.
There is no evidence that continuous home oxygen therapy has a long-term benefit if it is administered to patients with COPD that only have a nocturnal decrease oxygen pressure or induced by exercise. Oxygen is not addictive or toxic, so it is very important to use it continuously as prescribed by the doctor.
Home mechanical ventilation (HMV) is a type of ventilation that can be safely used outside the hospital, and is used to boost, or even replace, spontaneous ventilation.The administration of oxygen is passive, that is to say, it offers a higher oxygen concentration that the patient inhales with their own effort. In mechanical ventilation, the different types of devices actively assist spontaneous breathing.
To carry out HMV, an apparatus that generates the airflow (called a ventilator) has to be used, as well as a mechanism that connects the apparatus with the airway. In the majority of cases, this connection is achieved using a nasal or facial mask, or a mouthpiece. In other cases, this type of ventilation has to be carried out through a tracheotomy.
HMV improves the survival of patients with neuromuscular diseases and those of the thoracic cavity, as well as improving anomalies in gas exchange and the quality of life of patients with obesity-hypoventilation syndrome (OHS).
Its role in COPD is controversial and recent studies do not appear to show any improvement in survival. Its effects on lung mechanics, breathlessness or shortness of breath (dyspnoea) or the quality of life are still being studied.
Hospital at home is an alternative care program for COPD patients who suffer decompensations. There is evidence that shows that to treat COPD decompensations at home in well-selected patients is as safe as in hospital. The impact on the patient is very positive and also has a great impact on the health system. The absence of a competent carer or clinical instability contraindicates this alternative.
Substantiated information by:


Published: 20 February 2018
Updated: 20 February 2018
Subscribe
Receive the latest updates related to this content.
(*) Mandatory fields
Thank you for subscribing!
If this is the first time you subscribe you will receive a confirmation email, check your inbox