- What is it?
- Causes and risk factors
- Symptoms
- Diagnosis
- Treatment
- Living with the disease
- Research lines
- Frequently asked questions
- Team and structure
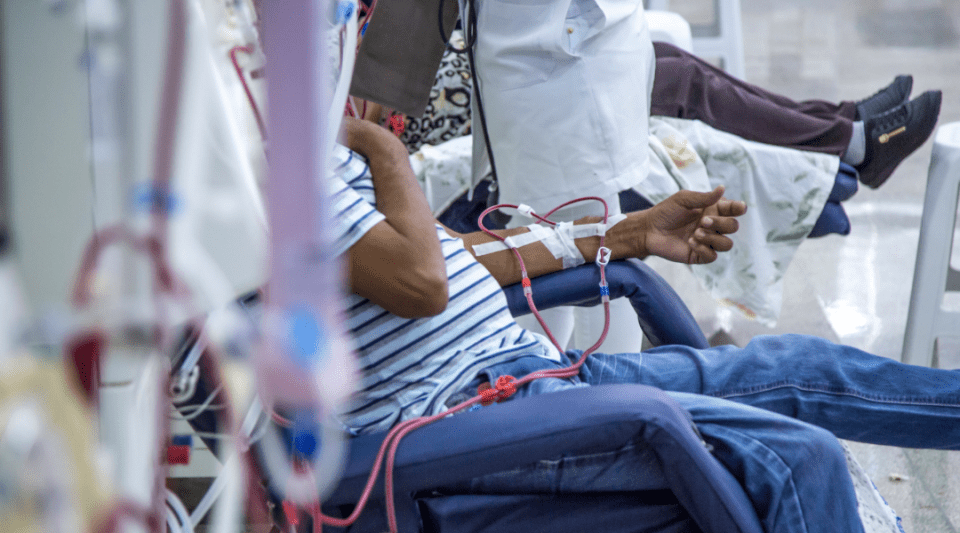
Living with Chronic Kidney Failure
Adopting a healthy lifestyle is an essential part of caring for people with Chronic Kidney Disease (CKD). Healthy habits help improve disease control, reduce the risk of complications—especially cardiovascular ones—and maintain a better quality of life in the long term.
The main recommendations are:

Do not smoke, as tobacco accelerates kidney damage progression and significantly increases cardiovascular risk.

Maintain a healthy weight through a balanced diet and regular physical activity. This reduces the burden on the kidneys and the cardiovascular system.

Control salt intake by limiting the consumption of processed, ready-made foods to support better blood pressure control and prevent fluid retention.

Maintain regular daily physical activity according to each individual’s capacity, to avoid sedentary behaviour and promote mobility.

Attend regular medical follow-ups, which allow early detection of potential complications and individualised changes to treatment.

Maintain a regular sleep pattern.

Take medication as prescribed.

Maintain open communication with family members and caregivers.
Commitment to these habits and ongoing follow-up by the healthcare team are part of a comprehensive, preventive approach to CKD, focused on overall patient health and well-being.
Nutrition is a fundamental part of the comprehensive management of Chronic Kidney Disease (CKD). The kidneys play an essential role in regulating the balance of water, minerals and waste products; when their function declines, dietary adjustments are necessary to slow the progression of kidney damage, prevent complications and maintain adequate nutritional status. An appropriate, individualised diet, supervised by specialist professionals, contributes significantly to symptom control and improves the quality of life of people with CKD.
Key dietary considerations for CKD include:

Energy intake: Adequate caloric intake is essential to prevent excessive weight loss, muscle weakness and malnutrition, especially in advanced stages of the disease.

Proteins: Protein intake should be adjusted according to the stage of CKD:

Sodium (salt): Reducing sodium intake is essential for controlling blood pressure and preventing fluid retention, oedema and cardiovascular overload.

Potassium: Potassium intake should be individually adjusted based on laboratory results and disease stage. In advanced stages, it may be necessary to limit potassium-rich foods to prevent hyperkalaemia.

Phosphorus: Intake should be moderated to prevent bone and cardiovascular disorders. Reducing consumption of dairy products and processed foods is recommended, prioritising fresh and natural foods.

Fluids: Fluid intake should be tailored to each patient, especially those undergoing haemodialysis, to prevent fluid overload and its complications.
Ongoing nutritional education and regular follow-up help in adjusting dietary requirements to disease progression and individual needs, forming an essential part of comprehensive, patient-centred care in CKD.
- Pukono: a tool to identify appropriate foods based on potassium and phosphorus content (Althaia Foundation, Barcelona).
- RecuerdaMed: helps manage medications, track schedules and detect duplications.
Regular physical exercise is a fundamental component in the comprehensive management of Chronic Kidney Disease (CKD). It helps improve cardiorespiratory fitness, muscle strength, mobility, sleep quality and emotional well-being.
Exercise also helps reduce cardiovascular risk factors, maintain functional independence and improve tolerance to activities of daily living for people with CKD.
Regular, physical activity adapted to the individual provides many benefits:
- Increased muscle strength and endurance, promoting mobility and independence.
- Reduced fatigue and improved functional capacity.
- Improved control of blood pressure and cardiovascular profile.
- Reduced risk of falls by improving balance and coordination.
- Improved mood and emotional well-being, reducing stress and symptoms of anxiety or depression.
Exercise has to be adjusted to the individual’s age, stage of CKD and clinical condition. In general, the following is recommended:
- Daily walking, ideally 30–45 minutes, with the pace adjusted to individual tolerance.
- Reducing sedentary behaviour by including activity into daily routines, such as walking upstairs or taking active breaks.
- Strength training 2–3 times per week, with simple exercises targeting major muscle groups.
- Aerobic activities, such as brisk walking, cycling or swimming, provided there are no contraindications.
- Medical assessment and supervision in frail patients and those with significant comorbidities or functional limitations.
Gradually introducing physical exercise in a safe way is an important part a comprehensive, patient-centred approach, contributing significantly to improved health and quality of life in patients with CKD.
- Haemodialysis: Do not apply excessive pressure to the arm where the arteriovenous fistula is located.
- Peritoneal dialysis: Do not perform intense abdominal exercises.
- Kidney transplant: Gradual progression and avoidance of early abdominal strain is required.
Sexuality may be affected in people with Chronic Kidney Disease (CKD) due to physical, hormonal and emotional factors. This is a common but often under-discussed aspect and an integral part of quality of life.
- In men: reduced libido, erectile dysfunction and hormonal changes.
- In women: decreased sexual desire, vaginal dryness and difficulty achieving orgasm.
- Common factors: fatigue, pain, body changes, stress and medication side effects.
The presence of catheters (peritoneal dialysis or haemodialysis) or surgical scars may lead to body image concerns and insecurity. Open communication with a partner and emotional support are important for maintaining a satisfying sex life.
Chronic Kidney Disease (CKD) not only has a physical impact but also involves significant emotional and psychological changes. Adapting to the disease can affect personal, work, family and social life, as well as experiencing emotions such as anxiety, stress, sadness or low mood.
Such emotional responses are particularly frequent at key moments, such as the initiation of dialysis, changes in treatment or after a kidney transplant. Recognizing and addressing them appropriately is an essential part of comprehensive care for people with CKD.
People with CKD may experience the following at different stages of the disease:
- Mood changes or increased irritability.
- Difficulty sleeping or non-restorative sleep.
- Loss of interest in previously enjoyable activities.
- Fear or concern about the future and about disease progression.
- A sense of dependence or loss of autonomy.
These experiences are not a sign of weakness and should not be regarded as “inevitable,” as they can and should be addressed.
There are various strategies that can help improve emotional well-being and the ability to adapt to CKD:
- Sharing doubts, concerns and emotions with the healthcare team, fostering a relationship of trust and support.
- Setting realistic, achievable goals in accordance with the individual’s situation and stage of life.
- Maintaining active social connections, preserving family and social relationships whenever possible.
- Engaging in appropriate physical exercise, helping to improve mood and reduce stress.
- Maintaining regular rest and sleep schedules, supporting healthy daily routines.
- Identifying and limiting repetitive negative thoughts, learning strategies to manage them.
- Seeking support from specialist professionals (e.g. in psychology, social work and nursing) when emotional distress interferes with daily life.
Caring for emotional health is a fundamental part of CKD treatment and contributes significantly to better adjustment, greater autonomy and improved quality of life.
People with CKD can travel, although planning is necessary depending on the treatment they are receiving. With proper organisation, most patients can enjoy both short and long trips.

Patients not requiring dialysis. They should maintain healthy habits, carry sufficient medication and have an up-to-date medical report. It is also useful to bring recent laboratory test results.

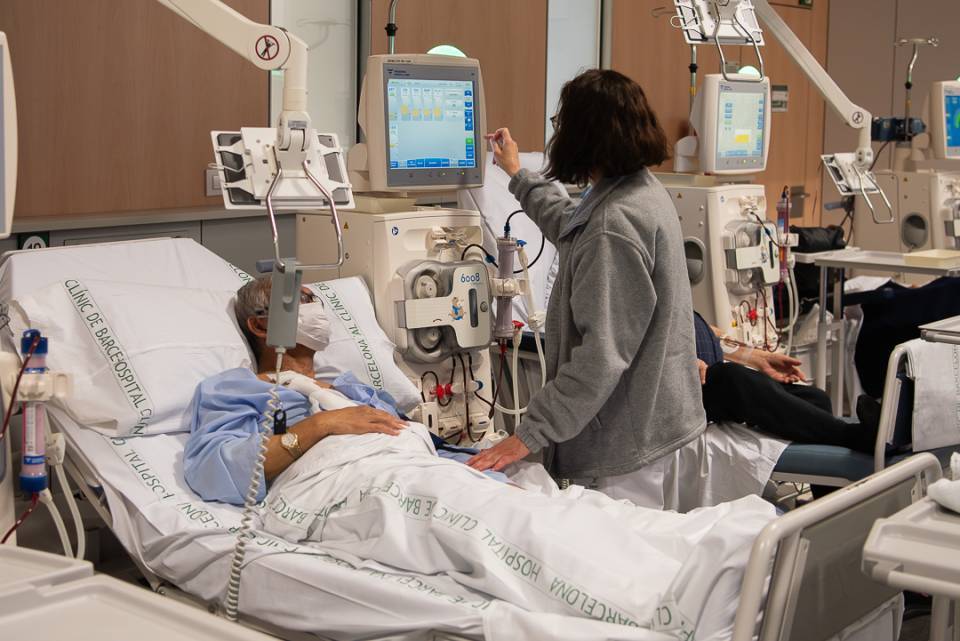
Patients on haemodialysis. They can receive dialysis at other centres with prior arrangement. It is essential to prepare:
- An up-to-date medical report.
- Recent laboratory tests (<30 days).
- The latest dry weight measurement (body weight after excess fluid has been removed through dialysis)
- Medication for the entire trip.

Transplant patients. Destinations with a high risk of infection should be avoided. Patients should carry sufficient immunosuppressive medication and an up-to-date clinical report.
Substantiated information by:







Published: 20 February 2018
Updated: 20 February 2018
Subscribe
Receive the latest updates related to this content.
(*) Mandatory fields
Thank you for subscribing!
If this is the first time you subscribe you will receive a confirmation email, check your inbox